Have you ever tried to watch a movie from the front row? Difficult isn’t it. Miserable as well. Today’s Medical education, with its over-emphasis on TECHNOLOGY and DIAGNOSTICS, can be a lot like watching a movie from the front row.
Because the practice of medicine is predicated on taking the body and dividing it, subdividing it, and dividing it some more, it tends to give student doctors a “front row” perspective of anatomy and physiology. Think about it; we have kidney specialists (nephrologists), heart specialists (cardiologists), nerve specialists (neurologists), butt specialists (proctologists), muscle and joint specialists (orthopedists), stomach specialists (gastroenterologists), arthritis specialists (rheumatologists), kidney specialists (nephrologists), mental health specialists (psychiatrists), etc, etc, etc, etc, etc.
Unfortunately, this model is out of date. It fails miserably as far as really advancing our understanding of the human body because you never really get to see the BIG PICTURE. For one, it cannot explain how the whole organism is greater than the sum of its individual parts. What do I mean by this? For instance, Hydrogen (an explosive gas) + Oxygen (a flammable gas) = Water (H2O), a liquid — the foundation of all life — that’s used to quench fire.
The problem with using outdated models that reduce and subdivide the body into increasingly smaller parts is that the ‘Big Picture’ is frequently missed — spend some time on our “Blog Roll” (right margin) and you’ll quickly understand what I mean. The movie ends without the student-doctor ever moving from the front row. And unless physicians are willing to step outside of “the box” that is their formal educational model (something they are encouraged not to do by THE POWERS THAT BE), the “Big Picture” is rarely grasped.
Doctors use this same philosophy and thought process when trying to explain the musculoskeletal system. Fascia is one of the best examples that I can think of concerning this phenomenon. Doctors frequently miss the forest for the trees because the doctors they learned from were taught by others trained in the same reductionist philosophy. Furthermore, they use books that show hundreds of pictures of individual muscles —- without ever really showing or explaining the fascia.
Go to virtually any anatomy text book and take a look. The fascia is almost always removed so that we can see the really “important” tissues underneath. Never forget that removed = ignored. And after all; if the medical text books are not talking about fascia, showing us lots of pictures of fascia, and EXPLAINING HOW FASCIA WORKS; exactly how important can it really be?
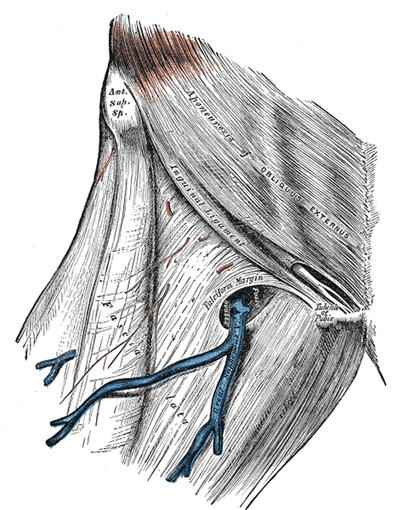
Because the illustrator for the famous anatomy textbook of all time (Henry VanDyke Carter) left the fascia intact in a large number of his drawings; most of the anatomical drawings on my site come from Gray’s Anatomy. Even though the first edition of his renowned textbook was written over 155 years ago, Henry Gray is still considered one of the greatest anatomists the world has ever seen.
f
fWHAT IS FASCIA?
Fasciae (plural) are the tough layers of fibrous, collagen-based connective tissues that permeate the human body. If you are a DEER HUNTER, you have seen fascia and know what it is. It is the thin, white, cellophane-like, membrane that wraps itself tightly around the muscles. Around here folks call it “Striffin” or “Silver Skin“. But there is far more to fascia than what is readily observed while butchering.
Fascia surrounds individual muscles, muscle bundles within individual muscles, groups of muscles, blood vessels, and nerves. It binds these structures together in much the same manner that plastic wrap is used to hold the contents of your Hoagie together. Fascia consists of several extremely thin layers, and is the tissue where the musculoskeletal system, circulatory system, and nervous system all converge. It extends from the top of the head to the tip of the toes, and like ligaments and tendons, contains closely packed bundles of wavy collagen fibers that line up in an organized and parallel fashion (PICTURES HERE). Subsequently, healthy fasciae are flexible tissues that are able to resist great tensile forces. Unhealthy fascia? We’ll get to that shortly.
Fascia forms a whole-body, continuous, 3-D matrix of structural support. Its connections extend to all fibrous (elastic) connective tissues, including APONEUROSIS, LIGAMENTS, TENDONS, RETINACULUM, joint capsules, organ and blood vessel sheaths, the epineurium (nerve sheaths), the meninges (spinal cord sheaths), the periosteum (sheath that surrounds bones), as well as the membranes that surround MUSCLES.
Among the different kinds of tissues that are involved in the body’s “elastic” framework (chiefly ligaments, tendons, muscles, etc); fascia has received the least scientific attention – probably because in most regions of the body it cannot be imaged with even the most technologically advanced imaging techniques such as MRI (hey, out of sight, out of mind). Nevertheless, fascia plays a major (albeit poorly understood) role in joint stability / instability, PROPRIOCEPTION, coordination, strength, joint motion, as well as PAIN SYNDROMES of all kinds. It can even be involved in ANY NUMBER OF DISEASE PROCESSES.
f
Critical Functions of Healthy Fascia:
- It binds and holds muscles together compactly.
- It ensures proper alignment of the muscle fibers, blood vessels, nerves, and other tissues within the muscle itself.
- It transmits forces and loads evenly throughout the entire muscle.
- It creates a uniformly smooth surface that essentially “lubricates” the various surfaces that come in contact with each other during movement.
- It allows the muscle to change shape as they lengthen or shorten.
f
d
Collagen
Collagen is the building block of all connective tissues. Some collagen-based connective tissues like bone and most cartilages, are part of your body’s load-bearing framework. Their purpose is to withstand compressive forces, while grossly maintaining the body’s shape.
On the other hand, you have the Elastic, Collagen-Based, Connective Tissues, whose chief job is to resist the tensile forces that are constantly trying to pull joints apart whenever movement or muscle contraction takes place. These tissues don’t need to be able to bear heavy loads, but instead, must be able to stretch and elast (at least to a slight degree) while resisting tearing. Of these “elastic” collagen-based connective tissues, fascia is the most elastic.
As long as the individual collagen fibers that make up the fascia, are aligned in parallel fashion to each other, the tissue is stretchy and elastic (think about long hair that has been combed out. If you run a comb or brush through it, it glides — smoothly and unrestricted.) But what happens when fascia is injured?
When fascia is stretched beyond its normal load-bearing capacity, it begins to tear. Bear in mind that these tears are so microscopic that they never show up on an x-ray, and only on rare occasions will they show up on an MRI (possibly in the Plantar Fascia on the bottom of the foot — HERE). Fascial tears can be caused by sports injuries, repetitive trauma, car wrecks, postural distortions, falls, child bearing, abuse, etc, etc, etc. Oftentimes people have no idea how they ended up with Fascial Injuries, which often result in FASCIAL ADHESIONS (sometimes known as “FASCIAL DENSIFICATIONS“).
Whenever a muscle is impacted (contact sports, falls, abuse, etc) or overused / injured (lifting weights, running, over-training, heavy or repetitive jobs, etc), collagen microfibers form in between adjacent layers of fascia to bind them together so that the muscles can heal. These microfibers are sort of like nature’s internal cast.
Unfortunately, these “casts” do not automatically go away after the area has healed, and they tend to accumulate over time. This means that over time, the elastic, collagen-based tissues (particularly muscles and fascia) get increasingly stiffer and less stretchy. If you are over the age of 35 or 40, you have likely figured this out the hard way!
Think of the collagen found in fascia in terms of a Slinky. In normal collagen, there are waves. A slinky is no different. The coils of a slinky act like waves and give it the ability to elast and stretch in response to tensile forces. As long as the load is not too great to overcome the tissue’s tensile strength, it can spring back —- and things are peachy.
However, if the most elastic of the collagen-based tissue (fascia) is forced to resist more tension than it can handle, tissue failure begins to occur. The tissue increasingly loses its ability to stretch and elast. Think of this as a slinky that has been stretched out to the point of failure. The material has not necessarily broken, but it has been stretched far enough that it is not going to “spring” back like it should. This leads to tangles, which is a whole other problem unto itself. We have all experienced a mangled Slinky before. This is similar to a Fascial Adhesion!
FASCIAL ADHESIONS
UP CLOSE & PERSONAL
Bottom Line: If something causes fascia to exceed its normal tensile capacity, there will be a disruption or “micro-tearing” of individual collagen fibers. This in turn leads to fascial “scarring” and adhesion / restriction.
Think of fascial scarring in another way. Put both of your hands flat on a table in front of you, and slide the fingers of one hand back and forth between the fingers of the other. This is similar to the way fascia works, and is what gives all of the elastic connective tissues including fascia, ligaments, tendons, etc, an incredible amount of stretchiness and flexibility. Normally functioning fascial membranes are not only arranged in a very organized and parallel manner, but if you were to look at them on edge, they are flat and smooth —- like a piece of paper.
Once fascia is injured (stretched, pulled, torn, etc.), the microscopic fibers become disrupted and deranged. Instead of fibers running parallel to each other in an organized fashion with their normal degree of elasticity / flexibility, the fibers now run every possible direction in all three dimensions and have an extremely diminished amount of organization and elasticity. Interlock the fingers from one hand with the fingers from the other, only now do it with the fingers pointed in all directions. Now try to slide the hands back and forth. See the difference in flexibility?
Also notice that when the fingers are interlocked randomly, they will no longer lay flat on the table. Facial Adhesions act in much the same way. When fascia is injured, individual fibers run every which direction, in all three dimensions. This means that the fascial membranes no longer lay flat like a piece of paper. Instead, they are more like a wadded up or crumpled piece of paper. Unfortunately, injured fascia frequently heals in this tangled, twisted, and wadded-up manner.
We can also think of this fascial scarring and adhesion in terms of hair. Remember our example of well-manicured hair that a comb or brush glides through easily? Now think of the exact opposite. Think of a HAIR TANGLE. What happens to hair that is not well taken care of, or was slept on wet? Instead of the individual hair follicles lying parallel to each other in a neat and orderly fashion, they become tangled with the individual hair fibers running in every conceivable direction. The result is a tangled mess —— a ball of hair that takes forever just get a comb or brush through it. “Hair balls” can be so restrictive that just trying to get a comb through it, pulls and causes great pain. This is even more true with fascia. Most people are unaware that……..
FASCIA IS THOUGHT TO BE THE MOST PAIN-SENSITIVE TISSUE IN THE ENTIRE BODY
When the organization of the parallel collagen fibers of fascia are disrupted by injury, a host of really bad things begin to happen. The first thing that occurs is restriction of joint motion. Understand that if you have tissue restriction, you will automatically have some degree of loss of normal joint motion in the corresponding area(s) of the body. Also understand that loss of normal joint motion virtually assures you that sooner or later there will be pain —- even if you are not yet experiencing pain. Unfortunately, pain is not the only thing associated with loss of normal joint motion. One of the biggies is degeneration.
Loss of, or abnormal joint motion, is the known cause of localized joint degeneration. When I speak of localized joint degeneration, I am talking about things like calcium deposits, bone spurring, and loss of articular cartilage or disc height. Degeneration is a great example of a “vicious cycle“: Loss of joint motion causes joint degeneration —– and joint degeneration causes loss of normal joint motion. Repeat. As this cycle spins around and around, it causes pain.
STOP! Think for just a moment. Pain is frequently nothing more than a by-product of the vicious cycle. This is why pain pills and other similar measures (drugs), mask symptoms of Chronic Pain (ineffectively, I might add) without ever addressing its underlying cause. And on top of this, some of the most popular musculo-skeletal drugs (corticosteroids for instance) actually increase the degenerative effect (HERE). In many cases of Chronic Pain, the underlying cause is Subluxation, Fascial Restriction, and microscopic Scar Tissue.
Think for a moment how problematic this whole scenario is. Fascia is the single most pain-sensitive tissue in the body —— yet it does not image well with even the most advanced imaging technologies such as MRI! What does this mean? Those of you who have dealt with Chronic Pain long enough, know exactly what it means!
It means that when you go visit various doctors (orthopedists, pain specialists, neurologists, etc) they run all sorts of tests, and then look at you as though you are crazy. Or maybe they look at you like you’re a drug seeker, or trying to get Social Security Disability. Or maybe they just chalk it up to hard work and too many sports. Or maybe they just tell you that you have “arthritis” or “Fibromyalgia” just to get you out of their office. Or maybe they used that old and trusted standby, “After all Mrs. Smith, you just aren’t as young as you used to be.”
Whatever the case, the result is almost always the same. A blank stare and the recommendation for more pills —- or maybe even Corticosteroid Injections. The latest trend for Chronic Pain patients involves putting them on SSRI’s (anti-depression drugs) while trying to convince them that their Chronic Pain is the result of Clinical Depression; when just the opposite has been proven to be closer to the truth. (Chronic Pain is far more likely to cause Depression than the opposite).
Oh, and how about your doctor kick you a few more times while you are down. Scientific studies have repeatedly shown that beyond the wide array of side-effects to the kidney, liver, and heart; both NSAIDS, and cortico-steroids actually deteriorate collagen-based tissues —– severely and rapidly. This is why doctors will ration the amount of cortisone you can have, even if it helps your pain.
The Journal of Bone and Joint Surgery published a study over a decade ago that said if a person has more than one cortico-steroid injection in the same joint, over the course of their lifetime, their chance of developing premature deterioration of the affected joint is (gulp) 100%.
EFFECTIVELY HANDLING
FASCIAL ADHESIONS
The question always comes up, “If fascia cannot be imaged with advanced techniques such as MRI, how in the world does a chiropractor from the rural Ozark region of southern Missouri image it?” Plainly stated; I don’t. I examine the areas that I believe to be affected by Fascial Adhesions (15 years of experience has helped me know what to look for), and I start treating. Every year I get more proficient at knowing what to look for, finding it, and fixing it. What am I using to fix it? Glad you asked. I simply call “TISSUE REMODELING“.
WARNING
BRUISING AHEAD
Because our “Tissue Remodeling Treatment” consists of actually breaking the Fascial Adhesions and subsequent tissue restrictions that cause so many symptoms, there is often some bruising associated with the technique. Microscopic scarring is dense, inelastic, random, and unorganized tissue —– not what anyone really wants. If you have been paying attention, you are aware that scar tissue is not exactly an “optimum” situation. Nonetheless, scars (even the microscopic kind) are living tissue with a blood supply.
This means that when I “break” the adhesion, I also break the blood supply. There will be some internal leaking of red blood cells from the scar’s capillary bed into the surrounding tissue. Please don’t panic. In plain English, this means that you will have a bruise. When I break Fascial Adhesions, it is not uncommon that this bruising can be really really (really)ugly. Don’t worry — it really is OK. See our BRUISING & PICTURES PAGE. You can also visit our VIDEO TESTIMONIAL PAGE as well.
Although there are people out there doing similar things, I have yet to find anyone doing things quite like I am doing. This is why our results (click on the link above) are so radically different than those that most others are getting.
CONCLUSION
Fascia is the fabric that it woven throughout every part of our body to hold us together. Perpetually disregarded by the medical community as “unimportant” (hey, after all it does not show up on MRI’s), fascia is beginning to take its rightful place at the forefront of both cutting-edge medical research and cutting-edge treatment (particularly in the field of Sports Injuries and Chronic Pain Syndromes). It should! Fascia is arguably the most prevalent connective tissue in the body.
Other than the nerve system, is there another body system that CONNECTS THE DISTANT PARTS OF THE BODY TOGETHER in such an intimate manner? I say no! Fascia covers the body from the top of the head (Epicranial Aponeurosis) to the bottom of the feet (Plantar Fascia), and everything in between.
When there is a tightening or restriction of the fascia in one place, it can cause pain and dysfunction in distant and seemingly unrelated locations. And the kicker is that problems in the fasciae not only cause pain, they cause the nerve system to misfire. As you can imagine, the problems associated with a misfiring nerve system are many and potentially severe.
also be aware that what is true about fascia is true about the other Elastic, Collagen-Based Connective Tissues as well. Yes, ligaments are injured and respond to treatment in a similar manner to fascia. We also know from medical research that an almost identical tissue model can be applied for the treatment and healing process of people dealing with certain tendon issues as well. This is good news because tendon problems are a leading reason for musculo-skeletal doctor visits —- and Chronic Pain.



I was injured in March while working in manufacturing. A heavy metal object fell on my thigh,knee,then ankle. My 1st hospital visit claimed contusion . A large knot with bruising formed on my thigh More knee pain came I returned for another visit and was told I had fluid on my knee, sprain or strain and instructed to do R.I.C.E, and a knee brace.With the knot being ignored, more pain came. Doppler testing was negative. An MRI was conducted
IMAGING FINDINGS OF PATELLAR MALALIGNMENT, CONSIDER PATELLAR TENDON LATERAL FEMORAL CONDYLE FRACTION SYNDROME.
PROXIMAL PATELLAR TENDINOSIS WITHOUT TEAR
DISTAL FEMORAL METAPHYSEAL LESION WHICH MAY REPRESENT A FIBROUS CORTICAL DEFECT, HOWEVER, THIS IS NOT FULLY IMAGED AND EVALUATED BY MRI. RECOMMEND RADIOGRAPHIC CORRELATION. DEPENDING ON THE RADIOGRAPHIC APPEARANCE,
3-6 MONTH FOLLOW-UP RADIOGRAPHS OR MRI IS RECOMMENDED FOR REEVALUATION.
PROMINENT MEDIAL PLICA.
From my thigh all the way down to my ankle has the feeling of a brick when I touch it. Could it be possible that all of this is From adhesions, fribrosis, untreated?
Hello Simphony,
It certainly could be, but almost impossible to say without looking.
sincerely,
Dr. Russ
Awesome. Thank you for this 👍🏻
I tore the fascia in my left mid back. I keep having episodes of excruiating pain that express as spasms. I’m scared and miserable. I have to work now. Also I’m a nurse. Is there any hope of treatment?
Hello Linda,
This is the sort of thing that typically responds almost instantly to Tissue Remodeling.
Sincerely,
Dr. Russ
HI DR, WOULD YOU SAY USING THE FASCIA BLASTER SOLD BY ASHLEY BALCK GURU SAFE ? PLEASE HELP. IM ABOUT TO BUY THIS PRODUCTS BUT WANT TO JNOW IF ITS SAFE FOR ME TO USE
Hello Susana,
That can be answered HERE.
Sincerely,
Dr. Russ
thank you Dr Russ, I did read this article before reaching out to you however I am confused if I should use this product or not. don’t know if I am releasing Fascia or breaking it. may sound dumb but there are so many mix reviews on this that I want to make sure I wont be destroying something I need in my body . please advice , I’ve read we need the fascia to hold the muscles together
Odds are, you’ll do fine as long as you go extremely slow to start with. However, I cannot take any responsibility for her product or directions on using it.
Thank you for putting fascia in laymen’s terms.
I have been using a tool to break up my QL, MY PERIFORMIS AND PSOAS.
The relief after 20 + years, ahhhhhh. I feel like I can walk, skip, run again.
Thank you.
Question tho, will I need to continually work those areas of my body so the fascia stays healthy?
Again, thank you,
Rose
Hello Rose,
Make sure to read my post on this very subject (HERE).
Sincerely,
Dr. Russ
Beautiful ! Thanks for this detailed explanation.
I studied myofacial release techniques in the early 90’s and have used this as the basis for my treatment understanding, whether doing massage, Gua sha, cupping or acupuncture. This is the basis for the way I explain the things that modern science has chose to ignore. Good job and keep these articles coming 🙂
Thank you for answering me the depth of my gratitude is unfathomable. one more question and I do have a rheumatologist referral now I’m calling tomorrow. The dense matted knots or ropes ranging in size
but specifically right now the matted knots are continuing to break loose and my neck is matted crunchy badly and now ball matted knots are floating around in my neck.
I also feel a band around my temporal lobe that tightens more frequently now. Can this be helped in time? I’m concerned about an aneurysm or the total takeover off my organs. I’m frightened and feel like any moment. Heart palpitations are allot more frequent. muscles sucked in by fascia.. Doctor after doctor And everything you say is right. The hospital gave me a steroid shot… Rapidly huh? I just wonder is there a body wrap that heats us up finding the fascia with the diagnostic ultrasound and maybe laser them? Not the first time I invented something before it’s time just interrupted by a slow squeezing pain. If inky a machine invented with DNA. Why would any one body part be ignored by vision by medical equipment? Can you make one I’ll be your huckleberry. If it’s not too late. I’m covered from head to toe in deep crunchy fascia and can’t find information on it. Long crunchy bands in my chest that scab through my skin. What’s it doing too my insides??? Should I demand a full body diagnostic ultrasound from rheumatologist?
Sighs I am overwhelmed badly
Thanks for your patience
Terah
They will never do a whole body ultrasound and most would have no idea how to interpret it if they did. Make sure and read this.
http://www.doctorschierling.com/blog/crepitus-rustling-leaves-and-other-interesting-bodily-noises
Sincerely,
Dr. Russ
Terha- check out enzymatic therapy! I am a therapist and also suffering from adhesions and have been doing my research! The enzymes help break the adhesions and soften the fascia. Also look at taking magnesium at night and cut out all bread, alcohol, and artificial anything.
Thanks Dani,
All things I have talked about over on my Doctor Schierling dot com site at various times.
Sincerely,
Dr. Russ
Where does fascia go when released in your body? Ever hear of mummified people? Of course you have. I’m fasciafied literally. I released my organs last night which effected my hip flexor and IT band. I can’t believe I’m alive right now I’m so banded and matted, the left side fascia took the direction vertically.
IT band pushed into my buttocks, twisted, knotted. I was paralyzing. I saved my life I hope. Orthopedic appointment tomorrow, first one ever.
Hello Terah,
The Scar Tissue / Fibrosis doesn’t really “go” anywhere. The whole purpose of breaking it up is to specifically remodel it toward functionality and motion.
Sincerely,
Dr. Russ
Dr. Russ,
I was diagnosed with a rare autoimmune disease a little over two years ago. It is called Eosinophilic Fasciitis. It is reported some people have a sudden onset while others like myself have a gradual display of symptoms. I am wondering if you have had any insite on it?
Hello Kim,
While I have nothing to offer you on EF specifically, I have dozens of amazing posts on autoimmunity over at my Doctor Schierling dot com site.
Sincerely,
Dr. Russ
Thanks for your articles, they are so helpful to me! Can you tell me (as someone who is looking for some aesthetic improvements) how to “sheer” excess fascia or knotted fascia on the upper thighs that causes saddlebags? Is there a specific stretch you recommend, or a tool? I’m very slim and exercise and this area is the bane of my figure.
Hello Penny,
My practice is only concerned with Fascia as it relates to pain and dysfunction. There are others who deal with the aesthetic aspects. Watch my blog over at Doctor Schierling dot com. Because of the huge number of similar questions, I am currently working a post about ABG and her FB device.
Sincerely,
Dr. Russ
Dr. Russell
Your articles have been most illuminating. They have given credibility to my own research into the injury I suffered over 10 years ago. I am very interested in obtaining your own opinion on my situation. I would greatly appreciate the opportunity to speak with you.
Dr Russ, can you help me I’m being squeezed to death by deep band after band and more layers of band and rock size ? Buried deeply around my abdomen, breast bone, lower abdomen.
That I break apart except that in my top ribs near breast bone that point is a …
It squeezed my buttocks so bad glued to my skin that it gave me painful saddle bags.
Saddled at puberty and I’ve been snared every since and I’m 49. Doctor after doctor and back surgery2in1day. That started because I tore fascia in my right hip that is lumpy thick only with chunks of fasci. And the doctor said it wasn’t my leg that I have 2 torn discs
Every symptom now makes sense. I couldn’t eat without it hurting, it was getting harder to swallow my food. I even a baranium (?) test done once
I keep self grinding massaging gnawing at my legs but when tonight I once again made some fascia release and I found a too tender to touch underneath it. I did notice a difference in eating my food afterwards.
I keep finding painful core triggers now. Now I’m worried.
For years and gets worse every year I paralyze more but I don’t know what I’m talking about. Even got a test for ms.
The pain is so bad I didn’t know I get a dislocated shoulder that oddly crispy popped back in after working on my legs.
I’ve always avoided my abdomen and as years passed I forgot about those injuries and blocked them. Wait I blocked my childhood is pain why? I had an appendectomy at 10. My conclusion is this and the pass out beat downs. Flailing fists connecting too me randomly everywhere. Willow switches picked by the kids and the parents take turns us leaving welts and blood.
Injuries, traumas, severe childhood abuse
It was only about 4 days I realized the bands went around my entire abdomen and started there horizontally and my pent and bent thighs started really breaking through.
Doctors don’t listen. So you can’t image fascia so don’t talk about it!?
They think I’m a hypochondriac even friends and family. It’s so bad it’s taken over my shoulders. Daughter thinks I’m crazy
So sadly.. Add more trauma I had a freak car accident ripping the steering wheel out of my right hand now lost full function with tennis elbow. Spinning on the freeway I hit my head on the window now that’s the shoulder that was dislocated. TBI, eyes still take turns focusing and refocusing.
Sadly insurance just lapsed. That accident wiped me completely out.
I made a new doc listen and I have an ortho appointment this coming up Friday.
Is he the right doc? How will they find fascia? Exploratory surgery? I’m scared. I was squeezed to death. I touched myself to death probably.
I cry all the time now I know why. Explains mood swings
You could email me if you want I feel like this is my last chance. I wheeze now and this explains why I have chest pains too. Huh?
Unfortunately, most doctors — especially ortho specialists — are not too up on this stuff. Make sure to check out this very short post (HERE).
Sincerely,
Dr. Russ
Has anyone here heard of or used the fascia blaster? Is it possible that after the fascia is “torn” or “released” that it can bunch up under the skin and collect water resulting in weight gain? There are A LOT of women that have used this at home device and experienced hormonal issues, weight gain, loose skin, etc. Anyone here have any insight about this?
Hello Gina,
I get a ton of questions about the FB. While I think it can be a great tool, there have been similar tools around for a very long time. Bottom line, I see a lot of folks getting good results with the FB, and some complaining of bad results. My guess is that the claims made about it outperform its actual performance. And as far as it’s ability to effectively deal with cellulite — there have been lots of products come and go making similar claims (Laser Treatments are currently one of the biggies). While lots of things seem to help temporarily with cellulite, the only thing I know of that truly makes a difference over the long haul is strength training / weight lifting (HERE) — even better if done in tandem with a Paleo Diet.
Thank you for the quick response! So… Is it possible that after the fascia is “torn” or “released” that it can bunch up under the skin and collect water resulting in weight gain? Or…what do you know about fascia that would indicate that it’s manipulation could result in weight gain or loss of skin elasticity/muscle tone?
It could be a hormonal thing, Gina, explained at least partially by THIS POST.
Sincerely,
Dr. Russ
Last night my acupunturist told me the pain in my forearm is casued by fascia. I have been suffering this pain or over a month. The pain keeps waking me up every single night. He gave me electro- acupunture with infrared and a massage…it was painful and its not looking good now, but guess what?, it went from a 10 to a 7…and that is good news!!. Thank you so much for the information provided. Hola from Tijuana, Mexico!
You are welcome Lola.
Sincerely,
Dr. Russ
Thank you for a great article. I am extremely curious what you think of the fascia blaster tool by Ashley Black. I have used it a couple times and did find it received some of IT pain. However, as I have been researching some users are complaining that they have gain weight, severe detox symptoms, and worsening of the esthetic appearance, but there are some who are seeing phenomenonal results. I just want to do my due diligence. Thank you for your time.
I just answered this question from someone else (Gina I think). Make sure to take a look at it.
Sincerely,
Dr. Russ
I called your office to seek help about 4 years ago I had a lifestyle lift at the time of the procedure when he stitched above my cheek I felt a pull of tension across my cheek and the stitch sounded like a crunch as I felt my face pull with tension visually there was a pulled to tight look to that side and it felt pulled tight from that day forward it hurt everyday I went back repeatedly and I said something was wrong he dismissed me however the gland there was bulged out under the pressure of the tension point everyday I wanted something to release but no 2 years later I had extensive dental work 2 days later the pain got extreme and then I felt a tearing from beneath the cheek and that relieved some lower jaw tension but at the cheek the tightest area dimpled in and when I smiled I could only feel my smile from the tension point in my cheek I went to a doctor he said probably a nerve but it just kept hurting now in the last year I have crohns disease and had severe weight loss and dehydration and my cheek pain started getting extremely bad so my saliva gland got obstructed and I was in agony 4 weeks ago at the tension point in my cheek I felt a tear at the side of my eye and it felt like the gland dropped down like it had be constricted in the the cheek tension point I kept feeling a pulling away around my eye and for head even up through my scalp it felt like the gland kept moving fluid up and then down under the point of tension on my cheek it felt like the continuous peeling back of my skin on my cheek finally the i finally got the gland unblocked and then everything changed again I could taste but the tearing away situation in face was still there it kept pulling back further I kept telling the doctor it feels like whatever attaches my face is tearing it’s been like a curtain bunched up and pulled back by my orbit and my cheek that tension point is gone now it’s like I felt the last part tear away from the top of my cheek I keep wanting to push my face forwarded because it feels wadded up it feels like it’s want pull up towards my scalp and ear they done test they act like I’m insane they send me to pain management they do mri and say there’s nothing and when I smile it’s off and I only feel my face from the pulled back curtain area it feels a abnormal like nothing from mouth to the pulled back area I read your article and had hope I’m desperate for help hoping you can help this has been a nightmare and pain medication is not good for my situation they make me nauseated and I really just want it to get better
Hello Rachel,
I responded with an email.
Sincerely,
Dr. Russ
I have had chronic pain all over for 10-15 years. I was diagnosed with fibromyalgia 12 years ago, but none of the meds did anything but put me to sleep. Last year and pain doctor that sees people with EDS and MS diagnosed me in 10 minutes with EDS hypermobility. I read about it and finally something makes sense. I’ve tried everything and nothing helped. This pain doctor hasn’t stopped trying to help me tho. Unlike all the other doctors that gave up on me. Do you think I should start doing it myself? I can’t afford another doctor. We had to take out a loan to pay off my medical bills. My husband has been amazingly supportive through everything. But we live on one income because I’ve been sick for so long. Thank you!
Doing some of it yourself is fine Gail. There are any number of ways to deal with this on your own. Be aware that EDS is a different animal and that breaking the adhesions may actually make you more hypermobile. Make sure to look at my posts on EDS.
Sincerely,
Dr. Russ
So what would you recommend for us EDSers? It would seem to me that breaking up adhesions would allow our muscles to be “released” so we could build more muscle for joint support, no?
I do treat people with EDS, I just go about it a bit differently.
Sincerely,
Dr. Russ
Hi!
I have recently been fused L4-L5-S1 PLF in the end of January and all went well to begin with and after 3 weeks I was able to walk for 45-60 minutes. After 4 weeks I began to get excruciating stabbing muscle spasms at the fused area which almost makes me fall as my legs fold. My surgeon sent me to an extra CT scan and said everything looked perfectly fine. I feel he is only interested in the spine and the screws he placed there and I would like to know how the muscles and the fascia work after fusion and if there is anything I can do to prevent the spasms ? I understand they cut through the fascia to reach the spine. How does this heal afterwards? I have been bed ridden for 4 weeks now with only little improvement and as soon as I try walking as little as 1/5 of a mile I get flare ups and am back on square one where my back feels weak and spasms from moving even at snail speed. Would this be normal after a fusion? The surgeon removed my spinosus processus and used for bone graft instead of getting bone from my hips.
If you could just shortly advice me if my muscle spasms are normal I would be very grateful ! Nor the surgeon nor my PT has been able to give me an explanation for the stabbing spasms. I feel like I get stabbed to death several times a day…
Best regards, Lena
Hello Lena,
This is certainly a timely comment as I am going to tackle this issue in a blog post in the next few days. Watch for it.
Sincerely,
Dr. Russ
My life was destroyed from being Rolfed, no lie!! But if you are spot-rolfed in a particular area it might help you. Just don’t go through the 10 session protocol.
Tragic story Gerald,
Unfortunately, I have seen this sort of thing before. Most people can tolerate “deep” work, but there is a group of people who cannot. The work I do is fairly intense, but I am not the “deep tissue” guy. Thanks for sharing and I hope you find some resolution.
Sincerely,
Dr. Russ
HI, I have been dealing with constant pain from 2 separate injuries in the oblique/abdominal/hipflexer/intercostal area for almost a year now. I have had every test in the book, cat scan, ultra sound, MRI, X-ray…and everything comes back as normal. Ive been to the ER because the pain at one point was so intense. I have been seeing a physical therapist who stims me, ultrasound, laser, sports massage and graston technique. Now i am currently doing ARP wave therapy. And the pain still doesn’t seem to be going away. Sometimes I wonder if I am dealing with fascial damage, muscle damage or both. And wonder why the pain isn’t going away. Any time I go online looking for answers, I come to your site, and find it extremely informative. I wish I lived in the area,(I live in the Boston area) because I would set up an apt. I was just wondering if you have any other suggestions on how I could possibly treat this injury/pain.
Hello Tanya,
Not sure if you’d seen these (HERE & HERE).
Sincerely,
Dr. Russ
Thank you for sharing this Gerald. I too, am trying to convey to others what has happened to me. It can also be an issue of ‘energetic’ compatibility and whatever ‘accumulations’ and ego issues a practitioner carries. I;d advice people to get out immediately if you get an unsettled feeling, before even a touch and not to accept (false) assurances. I was injured badly at a consultation only appointment with an osteopathic practitioner, when I asked my chiropractors replacement to not touch the injury and showed the scans report indicating precarious damage, i did not realize the danger involved in in what could have been an ego threat to her. She choice to hit directly into the injury with a tension gun at full force. I now have fascial issues from hip to top of head and nerve damage, in addition to the original injury… all from a consult.. careful out there, everyone. What we think of as commonplace can be dangerous, even at a consult , even with boundary in place, even with assurance. If the practitioner is not ‘guided’ in their practice, other stuff can influence. Peace to you, and thank you for the warning… I was considering it and am sensitive to treatment as Dr, Russ indicates … thank you doctor Russ for bringing all of this to light.. i live no where near and have taken repeated stress to C1-2 occiput and all that’s all up and in there .. all without informed consent, against agreement. It happened over twenty years ago with a massage therapist crossing a room and pulling my head up off my body was I was sitting, because he felt entitled to and wanted to show his technique.. though I said NO. – Not all in healthcare/healing arts are operating from balance, even when you are not there to be treated .. there is the potential for issue. Life and service has been greatly impacted by this and I am back to trying to build way to something like normal function… some say.. ‘karma’.. other ways through that vs offering bodies up as sacrifice…
Chronic Regional Pain Syndrome? A veteran friend has been dx. The treatment is disgusting drug protocol with little to no relief besides a zombie like painful existence. CRPS primarily a fascia issue?
Hello Lisa,
I wish CRPS were a fascia issue. Terrible stuff. It’s where your pain gets locked into your brain and plays on a loop. It’s like SYMPATHETIC DOMINANCE on steroids. I would look at the free journal, Practical Pain Management, as they have some good articles on it.
Sincerely,
Dr. Russ
Hi, im 25 and have adhesions from the face down to my feet. Jaws are tight abd hips are tight as well. I am constantly dehydrated and stiff. My face is sooo tight that it parts of it feels stuck and its annoyingly uncomfortable. What would you recommend? Rolfing maybe?
Thanks,
Chris
Hello Chris,
Feel free to browse THESE POSTS. However, make sure to read them in light of THIS.
Sincerely,
Dr. Russ
I’m 44 years old lady. I fall in my job due to wet floor, on the 07january 2017,they check me and my x-rays show no fracture but my muscles stretches since now I’m not right.
I have eosinophilic fasciitis and have no luck with any treatment what would you recommend?
I can’t help you directly Eric, but I might be able to help you with THIS POST.
Sincerely,
Dr. Russ
Please would you tell me what makes fascia tear, and can it always repair itself on its own?
Thank you
Sue
Make sure to read THIS Sue.
Sincerely,
Dr. Russ
Oh my god !!! Finally some sense, thank you, thank you, thank you. I just turned 39 with 2 small kiddies and feel so old , soooo frustrated with medical care, ive been diagnosed with polyarthritis and I’m on an injection for it, im in a world of total pain but they just keep saying fibromyalgia and sending me home, rheumo’s, pain management, neuros etc etc…you have just made my year!!! one question, if its systematic (I feel I have tendonitis in a few areas as well) and will reoccur often whats my best plan of attack?
Hello Katrina,
Make sure to read THESE POSTS.
Sincerely,
Dr. Russ
I had tried Botox. I requested it and paid cash. The neuro didn’t know what he was doing. It did not work. Never went back nor did he have any kind of plan. All he wanted to do was write me scripts for Percocet. He never wanted to investigate the problem. He made me so frustrated I just threw the script away and continued my search to find an answer. I didn’t know I had CD at the time. This dr has experience with Dystonia and insurance is paying. She is a physiatrist at Tabor Ortho.and the one who diagnosed me. She is awesome – took my records home & studied them. Wow!! One of a kind. I am going to stay with her a year. My first treatment did not work. She has been doing Tigger Point Injections in between to help learn what muscles are responding and ones that are not. She adjusts her Botox plan based on my feedback. I have had 4 TPI every 2 weeks. The TPI give me relief for about 4 days. This helps her to adjust the Botox plan. Now, that she has adjusted her Botox plan I am hopeful my second treatment in Jan will be more effective. After a year, if my results are not great I am going to see Dr Le Douix (sp) . He is a movement disorder neuro in Memphis. I have heard great things about him. It takes about 6 months to get an appt. Also, she believes my suprascapular nerve did not heal correctly after being released. She is treating that with Botox as well. Yes, I agree with you I believe Botox will be better than powerful drugs that interfere with your thinking! Thanks again for your interest.
Danita
Dr Schierling,
Thank you for your response. Your right I was difficult to diagnose because I do not have the obvious signs. I had thought I had CD for a couple of years, but then I would dismiss it because I didn’t look like the pictures. Some peoples muscles are like concrete, that would be me. We do not all look alike. I found a FB page for people with Dystonia called Neuronauts. I have learned so much from the people who have the disease. You will not like the treatment, but the best treatment for CD is Botox. For many people it has been a miracle. You can only receive it every 3 months. The dr starts with the lowest dose and then increases if the muscles did not respond. It takes about a year to get the correct dose and correct muscles. Thank you for wanting to be aware of Cervical Dystonia.
Happy New Year!!
Danita
Not against Botox for certain things — it’s way better than many other meds. For some reason I was thinking you had already done botox injections? For many people they tend to be quite helpful. The biggest problem I see (I always see the failures) is that it does not last very long — although it lasts much longer than my 12 hr treatment did). Again, keep me in the loop.
Sincerely,
Russ S
Hello! I am a 29 year old mother of 3. I have a four year old and 6 month old twins. Being that I am a personal trainer and fitness advocate, I bounced right back after my 4 year old. However, with the twins, I had an emergency c-section and developed pretty significant diastasis recti. For the past 12 weeks I have been in physical therapy to heal my diastasis. I have went from a 4 finger with to a 1.5 finger with gap in that time. However, I still have a significant “stomach bulge/mommy tummy.” Even though I have lost my baby weight, been exercising regularly, been eating healthy and have been super strict about completing daily physical therapy, the stomach will not bulge. Today, I met with a plastic surgeon and was told that I have “overstretched” my abdominal fascia and would need a tummy tuck to get my flat belly back. Needless to say, I am now extremely discouraged. Is this true? Will I need surgery to correct my abdomen? Is there a way that I can take part in fascia therapy to correct my core? I would appreciate ANY advice and help. Thank you in advance!
Sincerely,
LaTisha
Hello LaTisha, A diastasis is a split or stretching that occurs in the abdominal connective tissues, down the linea alba, that lets the muscles underneath bulge through when there is contraction in them. These are ultra common and rarely dangerous, however, they trouble lots of people. To the best of my knowledge, these cannot be fixed by what I do or by PT. Make sure to do no situps but concentrate on planks and similar.
Sincerely,
Dr. Russ
This sounds very similar to what my problem is. I have adhesions in my abdomen that basicallly completely impedes normal functioning of my abdominal and pelvic organs, particularly my bowel. It is not visible by any radiological exam.
I swim, stretch, eat healthy, give myself massage, etc. I would love it if there were some miracle cure for this fasciae in my abdomen. It seems the only “cure” is a laporascopic surgery to separate the fasciae that are stuck together.
And good luck getting that treatment unless you have fantastic insurance or a whole pile of money.
All the Drs I have seen want more tests, more pills. This is just a brushoff and another way for them to make money. Drugs and tests. The patient does not get better and the Dr gets paid off for doing loads of tests and prescribing drugs.
Hello A,
It’s all unfortunate. Make sure to read THIS. Also make sure you realize that unless you have a true genetic defect (most of what we call “defective” genes are actually EPIGENETICS in action), there are steps you can take so that at the very least, you start to control the issue. HERE is a summary for you to take a look at.
Best wishes A,
Dr Russ
Wow Where have you been -I’ve thought your thoughts -been told almost all of the “common” things to do. Thanks for sharing! Will be going to your sight to read more.
Glad it’s been helpful Jacquette.
Sincerely,
Dr. Russ
I am 34 and was in a car accident at 14 i know i have this problem all over my entire body have been rebuilding my body for 2 years can u help?
Tough to say Kenyanna. before you even think of coming to see me, make sure to read the post I put up a few days ago called Death by Fibrosis (over at my Doctor Schierling dot com site).
Sincerely,
Dr. Russ
I really liked this! I am a 53 yr young former massage therapist now with chronic pain myself – arthritis in several low back and SI areas, compressed discs, migraines, pelvic pain. Docs say fibromyalgia too. I would like to know your thoughts about adhesions causing some of this pain in the low back and pelvis. Could that be part of the problem due to surgery? uterus, Fallopian tubes, ovaries and gall bladder all taken out in one surgery in 2011 using laparoscopy and robotic equipment. I also lost both breasts due to cancer in 2008 replaced with silicone implants .Very little female hormones now and losing bone mass. Depressed. Please share your thoughts about adhesions deep inside the body and what can be done to find them then break them up without having to undergo surgery again. Is that possible? I would guess no. Thank you so very much for posting this highly informative article. I live in St Petersburg, FL.
The very first thing I would do Claudia is head over to my Doctor Schierling dot com site, go to the blog, and scroll down the right side of the page until you get to the category labeled “Inflammation”. Read it all as it will shed a great deal of light on all your problems.
Sincerely,
Dr. Russ
Claudia, due to health problems that our daughter is experiencing after having silicone breast implants in 2012, I was doing some research on fascial adhesions and came across this website and your comment. Please visit this website and read the information and watch the video by Dr. Susan Kolb. Our daughter had thyroid cancer and had her thyroid removed and subsequently lost a lot of weight. As a result her breasts needed to be somewhat “reconstructed” which is why she had small implants. I’m not suggesting that some of your symptoms aren’t the result of fascial adhesions but based on the research I’ve done it sounds like you may have symptoms that are the result of problems with your implants which is much more common then people realize. Typically the surgeon that put the implants in is not going to believe your health problems are the result of your implants so it’s important to have a consultation with a surgeon who understands the issues. Dr. Kolb understands the issues. I hope you can get to the bottom of your issues. There are many groups on Facebook where people communicate about this issue.
Thanks for bringing this up Joyce,
I remember the first woman I saw really messed up by her implants about 25 years ago. In the time since, I’ve seen it time and time again. These things leak and people first make antibodies against the leaking material, and then they start making them against self (autoimmunity). I have also seen lots of people messed up by plastic surgery in general (HERE). I always caution people to think twice about such procedures.
Dr. Russ
Hello Dr Schierling, I just wanted to give you an update on my condition. I came to you a couple of times for treatment. I always felt great when I left your office, but within a few hours my symptoms & pain returned. Every therapy I tried this was always my results. Recently, I have been diagnosed with Cervical Dystonia. There is no cure, and the best treatment is Botox for the muscle spasms. I am not sure if you are familiar with this disease, but a good description is on the Mayo Clinic website. I wish your treatment could have worked longer than a few hours. If I lived closer I would probably come in just to get those few hours of pain relief. Hope all is well and you are able to help lots of people. Just wanted to make you aware of Dystonia as most people do not have a clue what I am talking about. Many different neurologists were clueless. I found a great physiatrist who diagnosed me and is treating me. She actually took home 12 years of records & studied them. Wow!! Sincerely, Danita
Sent from my iPhone
>
I certainly do remember you Danita; from the Memphis area.
I’m glad you found out what’s causing your neck issue, but hate the fact I could not help you more than I did. I would not have come up with that diagnosis. I’ve seen a couple of cases over the years but they looked a bit different than yours — jerky movements and an obvious torticollis (BTW, I was not the one to dx them). Do me a favor and if you find something that truly helps you with this, let me know what it is as it will likely help me send the next person like yourself in the right direction. PS, because this is a brain-based problem, a Functional Neurologist trained by Dr. Ted Carrick might be able to provide some answers.
Wishing you well Danita,
Russ S
I have a severe nerve pinch feeling between the SI Joint and the musculature near the spine. I had surgery on my lower back and the surgeon found no nerve compression anywhere. I cant tell if the nerve is being pinched in the SI Joint and causing pain backwards up the nerve, or the nerve is being compressed by a fascia adhesion, and then the area down stream of the nerve is burning because of it. I guess a 3rd option would be a quadratus lumborum tear at the attachment level in the lower back, since I have bad pain at the classic referrals sites for QL problems. Would you be able to help me? I am thinking about scar tissue remodeling.
Hello Danny,
This could certainly be a Scar Tissue issue. Make sure to read my post on the Thoracolumbar Fascia and Back Pain as well as my post on SI pain. It is common for pain in that area to be the result of Fascial Adhesions.
Sincerely,
Dr. Russ
Hi Dr Schierling,
Thank you for responding :). I’m actually on Day 27 of Whole 30 hoping it might help with my pain issues. I’ve been following the diet closely and have not cheated. I’ve noticed a huge difference … I don’t feel bloated anymore, I’ve lost inches everywhere (I still haven’t weighed myself), I’m sleeping better and my skin and hair look better. However, I haven’t noticed any difference in my pain.
The first symptom I get before I go into a full on whole body flare is carpal tunnel. A year ago I got carpal tunnel so bad that I had to get cortisone shots and my neurologist talked about surgery. At the same time I had started getting knee pain so I told my neurologist I thought this might be something systemic and I needed to talk to my rheumatologist. So I travelled to see her at Johns Hopkins and she confirmed that I was having a flare up and she put me back on prednisone.
When I was initially diagnosed with EF I was told that this disease tends to go into permanent remission after treatment and there would be no flares. I was also told that, although my muscles were being attacked, this disease never manifested into heart problems. Both of these things proved to be untrue with me. My doctors discovered a blood clot in my heart 6 months after my EF dx and determined that the clots formed because of scar tissue in my heart caused by eosinophils. My dr theorized that if I had not been on a high dose of prednisone, the damage to my heart would have gotten worse and killed me quickly. So my dr tends to be aggressive with the prednisone.
I go back to Hopkins in a month and I had hoped the Whole 30 would have helped my pain (I still have carpal tunnel pain) so that I could get of prednisone for good. Unfortunately it hasn’t. The one thing I haven’t cut out is nightshades so I suppose that’s my next step.
Thank you for all of your thorough information.
This is super cool Kristi! What I tend to find is that Nightshades are often associated with pain. I would cut them out for a couple of weeks and see what happens.. Because EF is autoimmune and because autoimmunity is so linked to Gut Health and past history of antibiotics, make sure to read my stuff on FMT as well. If nothing else, you will find it extremely fascinating.
Sincerely,
Dr. Russ
This is an important topic.
How can we locate journal articles that address the treatment of myofascial adhesions in cases of thoracic strain? Is there much research in this area?
Is there a separate or additional diagnosis term or code for thoracic strain that includes myofascial injury? Or is “thoracic strain” a large category that includes myofascial adhesions and other dysfunction?
Pubmed is the best place to start.
Dr. Russ
I have symptoms of pudendal nerve entrapment for at least 15 years, I had the pudendal release surgery twice with no worsening or improvement. Had minimally invasive lower back surgery for some foramanial narrowing, facet hypertrophy, no improvement or worsening. I think I have either a carpal tunnel type situation with the sacral/l5 nerves, or that my left sacrollliac joint is totally messed up so bad that it is referring pain to the low back, hip, piriformis, pelvis, privates, and butt. I am trying stretching, nerve flossing, and dry needling with a PT but the sexual pain/dysfunction/lower back pain or sacroilliac pain is not going away, in fact the more aligned my pelvis is, the more pain I have. Have you run into a case like mine?
Hello Charles,
I do not do pudendal nerve entrapment as I have never had good results with those people. Not sure why aligning the pelvis would make things worse.
Sincerely,
Dr. Russ
Sacral rami innervates the SI Joint, perhaps damage to the SI Joint would explain the sacral pain?
Yes, but the real question here is whether you believe you have “damaged” your SI.
Sincerely,
Dr. Russ
I have a lower lumbar fusion because of scoliosis and disc degeneration causing a lot of pain and movement. Now, 3 years later, I have a bulging disc right above the fusion and the pain is awful! It feels that my muscles are literally TEARING when I’m sitting, standing, or even lying down! My entire left leg is numb, with shooting pains going through it, and the constant achiness and fatigue. I’m sure the doctor is going to want to do another fusion if there’s instability in addition to the bulging disc. Any suggestions? I”m literally dying every day with this pain!
Hello Barbara,
Unfortunately, after fusions, people have problems with the joints above and below. The best thing I would recommend is my post over at DoctorSchierling dot com on the Thoracolumbar Fascia, Chronic Pain, and how to heal your own back.
Sincerely,
Dr. Russ
I recently (couple months ago) started a Pilates class that does tennis ball work for the feet to try to break up the fascia. I feel like I’ve opened Pandora’s box. Where there was no pain, now there is pain with every step. Is there a period of time it will hurt while it’s in the process of breaking? or have I injured it? It usually feels better after a good massage (me rubbing my feet in the spots they hurt). I must say that I have a horrible back (bulged the L5/S1, ruptured the L4/L5, scoliosis, etc. I get craniofascial (spelling?) and myofascial work about once a month… I will add that the majority of the pain is the in arch.
Hello Courtney,
Tough to say what you did here. The problem could be actually coming from (or highly contributed) your back. Have you tried inversion? Great modality for most disc problems. Make sure you go easy like I talk about on my site.
Sincerely,
Dr. Russ
I have been treating my own fascia restrictions for years now. I caused myself severe pain in the neck shoulders and head from sparring for so many years. Doctors wanted to give me pain meds by in my heart I knew that wasn’t the problem. I felt like my neck was in a tissue turtleneck that was choking me . I had hellerwork done, cranial work done, chiropractic, I do bikram yoga, I hang outside down, I put my neck in traction and mostly I manually break down the tissue between the joints in my jaw, neck and skull. It hurts. I hear and feel it break. But the more I do the more pain relief I feel. I sometimes wonder what other people do. Just take opioids for the rest of their lives? I couldn’t live like that and people give me weird looks when I tell them about what I have done to help myself. I feel sorry for them. So glad you do the work you do!! Great blog post!
Thanks for the Kudos Eve. I wish you the best.
Sincerely,
Dr. Russ
My mother has copd- i understand that damaged fascia is not the cause, but i wondered if it may aggravate her symptoms? She had a bad fall when she was 8, has had numerous chest infections that have resulted in terrible coughing bouts, etc., all of which must have affected the fascia somehow.
Absolutely Jaq,
Anything that causes restriction of the thoracic cage (rib cage) will to some degree prevent the ribs from expanding. When you can’t properly expand the lungs, breathing becomes increasingly difficult. As the rib cage expands (pigeon breast appearance common with COPD & emphysema), breathing becomes even more difficult. It really is a terrible vicious cycle.
Sincerely,
Dr. Russ
Hi Dr – I have had cramps and tightening in my calf muscles ever since I had a deep tissue massage a few months ago. I had the massage, which I didn’t know would be ‘deep’, for tight Achilles. The physiotherapist was very aggressive in the massage and for weeks after I was in pain. My symptoms seem to suggest fascia damage? Have you ever heard of this? I’ve read about compartment syndrome and i have those type of symptoms now.
Thanks!
Hello Aaron,
Very tough to say without examining you (CS). I have seen intense massage cause issues with people before.
Dr. Russ
have been in 15 car accidents since 2000.. some not so bad & some just awful. Never a broken bone, thankfully. But I live in constant, chronic pain at 36yrs old!! I’m a single disabled Mom & need help. I’ve done every therapy I’ve been sent too & tried every drug possible. I’m tired of being looked at as crazy & a drug seeker as well. I know I have other things going on like disc herniations, etc.. & being labeled as having “fibro” no1 believes U. I have been failed by the medical community & it sucks. I was once a thriving dental assistant. It is depressing living on a disability wage being a single parent & having chronic pain, however I’m not depressed! I’m in MA & if U know a professional I can see for this out here that’d be great.
Hello Jessica,
That’s averaging one MVA per year! I do not know anyone in MA, but I would suggest you go to my Blog and read the article I wrote on ‘Creating Your Own Exit Strategy’.
Sincerely,
Dr. Russ
I believe I might suffer from fascial tears/adhesions. I injured my back at work 4 months ago. 2 bulged discs, arthritis, stenosis and sciatica pains. Ive taken all the pills they gave me, completed physical therapy and I’m still in pain all day everyday.
After looking at an anatomy book with my physical therapist and seeing where the fascia is in the lower back, I really believe a lot of my pain stems from there. I’m doing work conditioning therapy now. They want to put me back to work even though I’m still in pain. I’m only 32 and I feel that’s too young to be in this condition.
I’m really glad I came across this article. Now I have some good questions for the doc and therapist
Glad to be of help Chris!
Dr. Russ
Hi Dr. Schierling,
As an occupational therapist, I recently tried some myofascial release techniques on a young patient who has been suffering from intractable back pain for years. Some nurses actually accused him of “drug shopping.” I could tell from his non-verbals he was indeed in pain. I did about 30 minutes of myofascial release and the look on his face changed completely and his pain lessened significantly. This reduction in pain enabled him to become much more functional. This treatment worked by changing the root cause of his pain, after drugs and other palliative treatments, like e-stim failed. This motivated me to use it on my fiance, who has severe degenerative disc disease. After 30 minutes, his pain went from a 7/8 (on meds and anti-inflammatories) to a 3/4 without any other intervention. He actually felt less constipated afterwards as well. I am a huge believer in this, after taking the John Barnes myofascial release course, but working in an inpatient setting with elderly people, I rarely get to use it. For anyone with chronic pain… try any approach that addresses pain on the fascial level. If it can help to address the root cause of your pain and minimize the reliance on pain meds (with exception of NSAIDS), you will be better off!!
Thanks Heather,
I have a very cool article right up your alley (its on my blog) called CHRONIC LOW BACK PAIN AND THE THORACOLUMBAR FASCIA. You are absolutely spot on as far as wanting to keep your patients off of drugs!
Sincerely,
Dr. Russ
Hi Dr.SCHIERLING I have been dealing with an oblique strain for 2 years now. It has gotten better only due to me babying it and not engaging in activities I love such as biking, running, hiking, weight lifting you name it. I pretty much feel like no one has a solution for me other than to take it easy. I received an MRI and they saw nothing other than mild Diastasis Recti (I had never been pregnant at that time). I am also 4 months pregnant. It seems like that hasn’t affected my condition much. I read and enjoyed your articles about fascial adhesions. Just hoping SOMETHING can help. I can’t decide whether to forever baby my injury or be in pain constantly. Do you have anyone you recommend in San Diego, CA?
Hello Meagan,
Thanks for the props concerning my article, glad it was helpful. As far as anyone in San Diego, there should be someone there who can help, I have no idea who. Honestly, your issue should be a relatively easy fix.
Sincerely,
Dr. Russ
This information is amazing. My 14 year old daughter and I have Ehlers Danlos. My daughter is quite severe and in constant chronic pain that very little helps. The pain in her hips is so bad that walking is difficult. we have tried loads of things o help her such as massage, float pods, physio both in and out of the water and still she is in terrible shape and its heart breaking to see a child who was once extremely active and carefree struggling just to walk.
Hello Tasha,
ED is different than Fascial Adhesions. Make sure to read my article on ED over at my Doctor Schierling dot com site.
Sincerely,
Dr. Russ
Excellent explanation for how fascia works and how all its connections can affect each other. I so wish doctors could really understand all this! Being a person dealing with chronic pain for so many years and no solutions just a bunch of typical tests, X-rays, MRI’s. Never a solution because probably the one thing that was never studied has just been constantly ignored 🙁
Where can i find a doctor to help me? I have been down in chronic pain for over 3 years. It is my entire back, butt and legs due to unreal muscle spasms. All of this came from a nasty fall.
No idea where you live?
Dr. Russ
I need help 😞 no one will help me … I’m reaching out I need to be seen and need treatment immediately. I’m 28 and feel like 128 .. if you can help me please contact me .. plz
Hello Ericka,
The only way I even have an idea of whether or not I can help you is for you to go to the contact page on my Doctor Schierling dot com page and send me a history. If I think I can help you, I’ll let you know. If I think you need an approach that I don’t offer here, I will try and point you in the right direction.
Sincerely,
Dr. Russ
I am a boxer and received a wicked liver blow that sent a force so powerful from the of the torso out through the front of the abdomen which happened to explode my fascia on the way out. I thought it was a cracked rib at first, then the muscle, & after 21 days it was still agonizing. It was a very studious massage therapist instructor who determined the damage to the fascia and began some therapy. No one else could tell me what I had wrong. I just hope I recover soon so I can have my pro boxing match this November. Thank you for this informative article. My boxing coach is among the best in the world with 3 decades in the sport and never had had or seen this injury before.
Robert Vega Jr.
Hello Robert,
Glad you found the right person to both figure out what was wrong with you and fix it. Wish you well in your next fight. BTW, my favorite boxer of all time was Sugar Ray Leonard. The fights with Roberto Duran and Hitman Hearns still resonate.
Sincerely,
Dr. Russ
I was diagnosed with Chronic Myofascial Pain Syndrome in 2002. I also found out I had Lupus SLE & Discoid, Fibromyalgia, Osteoporosis confirmed via bone density test. I was told that my fascia was hardened and oxygen could not pass through and get to my muscles. A lot of things from my past now made sense but I sure wish I hadn’t become severely symptomatic in order to be diagnosed. Many more health problems have developed since 2002 and I don’t know if anything can help me but I’d be happy to hear any suggestions…I’m a happy person because I refuse to complain though I am 100% alone (my social is on-line) and It’s at the point of not being able to do basic house chores. So, that’s the initial diagnosis but not the whole story and I’m not on any meds except 2 pain pills a day.
Hello Pamela.
This is a tough case that sounds somewhat like what my sister went through. Unless someone can show me something about hardening fascia inhibiting the flow of O2, I will have to chalk this one up to the wild explanations that doctors provide people, hoping they never check it out. With systemic “hardening” of fascia or any tissue, there has to be a source of inflammation. Even in the case of “genetics,” most similar problems are driven epigenetically (check out epigenetics on my Doctor Schierling blog). Also be sure to check out my SYSTEMIC FASCIAL ADHESIONS page.
Sincerely,
Dr. Russ
Pamela,
I’m not a doctor, but I would suggest checking out a tool developed by Ashley Black called the Fascia Blaster. It has helped a lot of people to break up their “hardened” fascia. She’s on Facebook and youtube.
Good luck to you!
Wait! This happens to my WHOLE BODY!!! I’m CONSTANTLY pulling joint muscles in EVERY part if my body 1-3 times a week! It’s crippling to me! I gently rotate my neck to stretch it and I hear crunch, crunch, crunch like plastic wrap being smushed into a ball! 😫 -And it happens to my whole body daily… AND I “DO” live in the Ozarks!
Hello Robyn,
Not saying I could not help you, but you definitely need to read THIS first. It could be THIS as well.
Sincerely,
Dr. Russ
Please help I have myofascial pain
Hello Priscilla,
I have tons of stuff on this topic on my blog.
Sincerely,
Dr. Russ
Hi, I have a sharp pain in the outside part of my left calve. It is to the left of my shin. Do you think it is a torn fascia? It would cause me bad, sharp, pain while I run. If I try to lean forward after running it would cause a sharp pain all the way up my left side of my lower leg. What kind of treatment can I do? Can this be shin splints?
Hello Jano,
It could be shin splints but without looking at you, it’s impossible to say. However, I would point you to my Shin Splints page on this site.
Sincerely,
Dr. Russ
Wow! I had no idea. I live in Henderson, NV. I have this issue. How and where can I receive help?
No idea where Henderson is not looking at a map, but there should be someone in Vegas who could help you.
Sincerely,
Dr. Russ
Hi. I live in India. I had backache since last 3 months.all investigation s MRI, x ray, usg and CT were normal and I was really considered psychiatric patient…..your article helped me a lot…
to understand my pain which is actually facial tension.
Thanks for sharing Kinnari.
Dr. Russ
Thank you for this most informative article. I have recently been diagnosed with eosinophilic fasciitis which has caused my arms, legs and abdomen to harden and stiffen. I had terrible pain and selling for months before the doctors figured it out ( by way of a deep tissue muscle biopsy). I am now on prednisone (started on 60 mg and have come down to 45). I know cortisteroids are not great but they have taken the pain away so I can get through my day now. However, my doctors have no idea what else to offer me in way of treatment and I really worry about permanent damage with this. I ask them to refer me for some physical therapies but they are not sure what I should do. I find any aerobic exercise exacerbates the stiffness so have been doing mild stretches but they can be painful and I worry about tearing because I am so stiff.
Any suggestions would be greatly appreciated.
Thank you
Jill
Australia.
Hello Jill,
Super rare problem. I looked it up and saw that there were only 300 known cases since 1974. Best guess is that this is autoimmune. Because it is at least somewhat like Scleroderma, I would suggest you go to my Doctor Schierling dot com site, type in the word “Exit” to the search bar, and read the first article that comes up.
Sincerely,
Dr. Russ
Hi Jill … I was diagnosed with Eosinophilic Fasciitis in Feb 2012 causing hardening of my fascia and joint contractures. Like you I was initially put on 60mgs of prednisone and tapered down from there. This is an auto immune disease so I’m also on immuno suppressants (most likely I’ll take them for life). My stiffness and pain gradually went away over time on the prednisone. After almost 5 years I’ve never gotten back my full range of motion or flexibility. And I still have arthritic pain in my hands and get flare ups of severe carpal tunnel and knee pain, putting me back on prednisone.
My neighbor recently purchased something called a Fascia Blaster from Ashley Black that she uses for back pain. I read a testimonial from someone with EF who said it helped a lot. I ordered one but haven’t used it yet and am hoping this will get me off prednisone for good! I’ll be checking Dr Scheirling’s website too.
Hello Kristi and Jill,
Autoimmune causes of Facial Pain are extremely common (HERE). You would do well to deal with underlying causes rather than working the Fascia. HERE is how you go about doing this.
sincerely,
Dr. Russ
I have some chronic pain undiagnosed which is an almost constant burning pain under my right scapula. I have had chiro which helped and then massage for the stiffness. Now the pain is back just as bad as ever…could this be fascia or scar tissue ?
Hello Josh,
I could very well be Scar Tissue in your Fascia. Be aware that the medical community refers to such tissue as “Fibrosis” (fibrotic tissue).
Sincerely,
Dr. Russ
I would like to include this article in a yoga teacher training that I’m doing. I feel like this is an area in which yoga can make a big difference in a persons health.Please contact me or let me know where I can contact you to make a formal request. Thank you!
I have a contact page over at my Doctor Schierling dot com site. BTW, I am a big fan of yoga and have seen it help numerous people.
Sincerely,
Dr. Russ
I have been diagnosed with SI JOINT injury, also was told by a different work comp Dr, it was arthritis in my spine. I tried to lift a 38 lb monitor at work from the floor. I felt a pop and could hardly walk without major pain. I have pain in my hip, buttock and my leg and foot go numb. I’ve had PT, chiropractic, injections, ( the 2nd showed dye leaking out, they think from the ligament possibly being torn. ) nothing has helped. I have noticed on my buttocks, there is a pulled look on my injured one, where my pain is. If the fascia is injured or torn, or the ligament, would it show up on the outside as in a jacked up cheek?
Hello Peggy,
Leaking dye indicates a capsular tear. Sometimes they do surgery on these, sometimes they try to let them heal on their own. Be aware that there could easily be other problems as well (Fascial Adhesions or others).
sincerely,
Dr. Russ
Excellent article. Just had a therapeutic massage where she worked on my fascia along the iguinal ligament and hip flexor. Incredible relief to my lower back where the pain had nestled. I gained a lot of flexibility after just one session. Icing today after a 5 mile run. It seems as if though she is on the same page as you.
Fantastic Gary!
Dr. Russ
I recently saw a doctor who has recommended prolotherapy to treat fascia tears and connective tissue at the costotvertebral joint for my back pain. I was wondering if you had any thoughts on prolotherapy and its effectiveness to treat fascia tears or any complications it may have.
What I do is much cheaper and less invasive. I have seen prolo work, but in my estimation, not a good starting point for what you are describing.
sincerely,
Dr. Russ
Please would you tell me does all fascia in the body heal itself if torn badly.
Hello Sue,
Here’s the thing; your body will always attempt to heal an injury such as torn Fascia. The problem is that although it always heals with some degree of Scar Tissue, sometimes it heals with much more Scar Tissue than others. As you know, this can be problematic. Check out my blog for more information. Just this week I did a two part series on this topic.
Sincerely,
Dr. Russ
Thank you so much for this article; it was most informative. I have a family member who has a condition where her collagen is breaking down in her body. She is now using a walker to get around and simple tasks are very painful. Could bound fascia be her issue or something opposite bound fascia?
Hello Shi,
While her problem could certainly be Fascia, it is not the sort of thing I can help her with. She undoubtedly has some sort of chronic degenerative autoimmune or genetic thing going on (see my article on “Systemic Fascial Adhesions”).
Sincerely,
Dr. Russ
Dr. Russ,
I am so excited to have possibly found the cause of my chronic pain and also a little saddened by the reality I’ve wasted almost 10 years of my being treated for “FMS” just knowing in my mind, for this long, that it was something else. I’ve been on every antidepressant, pain pills and even Plaquinill now for 5 years, while having my eyesight deteriorate as a side effect.
I have visible lumps in between my shoulder blades, my whole upper back and neck are always, what I call,”crunchy.” I can hardly move in the mornings and lately I’ve begun to feel the burn in between my ribs and I’m constantly stretching my jaw open. I could go on for awhile…
How does one go about finding someone in my area to preform this type of therapy? Also, do you feel it would be a good idea for me to start the stretching program immediately?
Desperate yet hopeful.
Ginger (Thank you for your time)
Hello Ginger,
Not sure who you need to see in your area. As far as everything you have mentioned here (including Fibromyalgia or FMS) be sure to check out my DoctorSchierling dot com site as it is loaded with dozens of articles on these very topics.
Sincerely,
Dr. Russ
Hi Dr! This is very interesting information. You have me wondering and with many questions!
I had lung cancer 3 1/2 yrs ago and they came through my back and under my breast and separated my ribs. Then I received 7 fun weeks of radiation, burning a hole through my back.
I have extreme back pain ever since that pain mgmt drs call Myofacial Neuropathy.
What do you think, what shall I do? I want to exercise but it causes more pain. (My horrible breathing is my other issue! They took most of my lung)
I am medicated with three meds for pain plus the cymbalta for pain /depression, just as you mentioned…
God bless you and yours, Sir.
Thank You for all of this awesome info and your time its a blessing!
Sincerely,
Michelle
Hello Michelle,
While this could certainly be neuropathy (a common result of radiation), the “Fascial Adhesion” component could be much bigger than anyone realizes. Make sure you read my page on Rib Tissue.
Sincerely,
Dr. Russ
Lacerated my forearm 3 years ago. Severed the ulnar nerve and had to get a nerve graft. My arm healed but now I have a soft bulge around the laceration area when I flex and it always feels under pressure therefor causing numbness in my hand still. Anything I can do to fix this?
Hello Justin,
Tissue Remodeling might fill the bill. Go to my blog and look at my recent post about post-surgical Scar Tissue.
Sincerely,
Dr. Russ
Hello ! I have this around my mouth jaw and lips ! I can’t shut my lips. I had very bad trauma a year ago and it’s led to this I broke my jaw in 3 places , cracked my skull and broke all the bones in my cheeks behind my ears and nose. I can feel my muscles try to work but are being help so tight back . I can feel the fascia in my tissue right where it doesn’t want to move. Looks like I’m smiling 100% of the time. Please any advice I’m begging for it. All doctors here don’t know what it is and I think I do ! They never talked about this to me they just keep telling me to wait. Please help I think a year with no lips touching is long enough for me. Thank you Krissy
I have several articles about the face on my blog Krissy. Tissue Remodeling can be safely and effectively done just about anywhere on the face.
Sincerely,
Dr. Russ
Hello,
24 years old and over worked my hip, ending up with bursitis, so I stopped exercise for four weeks. On a whim, during the four week break, myself and some friends decided to play kick ball. I very stupidly did not think to stretch, especially for not having worked my lower body in four weeks, before and after playing. My quads, every time I lunge or do a kicking motion, feel like they are going to rip. I believe these are the fasical adhesions you were speaking of. Will a foam roller/ hand roller do the trick or will I have to get massage therapy to work out the adhesions?
Foam roller and stretching is always a good starting point for something like this. Be sure to take a look at my Hip Flexor Page as well.
Sincerely,
Dr. Russ
Thank you so much for the great information. I had a bad car accident 3 months ago and today a wonderful orthopedic surgeon looked at my CT scan and told me I have a thoracolumnar fascia hernia that is at least 9 cm wide! Oddly enough the person that read the scan said it was fluid from a hematoma. It has caused me so much pain! My question is how do we fix this? I’m being referred to a surgeon to talk about surgery. I can not sit without excruciating pain and even standing for long periods causes pain.
Hello Cathy,
Probably a surgical problem (HERE).
Sincerely,
Dr. Russ
Dr Schierling,
Hello I’ve been having pain radiating from my sternum to my upper left back for about a year now. I think it was from bench pressing because one day my chest popped while benching and the pain has gotten worst ever since then. My chiropractor said i had a rib out and popped it in but the pain still continues. My chest pops when I cough or sneeze sometimes. Is there anything I can do at home to fix this? Nothing seems to help.
Hello Timothy,
Doubtful you can fix this at home after a year. You could try wallering around on a foam roller.
Sincerely,
Dr. Russ
Hi Dr. Schierling,
Thank you so much for all of this information. I found this article when looking for more science behind issues with fascia. I am hoping you might be able to point me in the right direction as you have kindly done for others.
In my mid 20s, I was misdiagnosed and given several rounds of fluoroquinolone antibiotics, then my issues started, and early on I was diagnosed with “myofascial pain syndrome” and Chronic Fatigue Syndrome shortly after.
I do have a generic predisposition to collagen issues that I discovered later (was diagnosed at 38 with Ehlers Danlos Syndrome (EDS) Hypermobility Type, my 8 year old daughter was diagnosed as well).
I have also been diagnosed with Lipedema, a painful fat condition that affects lymphatics, and cellulite, had stretch marks as a teen and have a very prominent pear shape since then as well (though I am in the upper normal range for BMI).
The Lipedema doc said that EDS and Lipedema are related, and after seeing information about a manual tool to break up cellulite, I started looking more into fascia and wondered if targeting fascia might help to pull more of my issues together for treatment. With EDS, there is info about loose ligaments and tendons, even lax blood vessels, but I hadn’t come across the collagen/fascia angle before. I’ve had a good myofascial release once before (therapist then moved) and am having some success (though short-lived) with osteopathic manipulative treatment.
How do you think your Tissue Restoration technique or a similar technique would work with someone who has allegedly defective collagen? Would a connective tissue disorder be contraindicated, or possibly the prime target for this kind of therapy? What types of things should I consider before finding someone/something to help break up fascial adhesions?
Thank you for taking the time to read this.
TB
All I can say TB is that Fluoroquinalone Antibiotics and ED are a heck of a nasty combination (I am not familiar with the Lipedema). I have articles on my website (Doctor Schierling Dot Com) on all of these — at least half a dozen on being “Floxed”. Although I have helped people with ED, the Antibiotics are a whole other beast altogether — one that I don’t really have any idea what to do about.
Sincerely,
Dr. Russ
Thank you for your reply. I am getting a lot of great info from the articles on your website. I think I will just take any fascia work slow and see how my body responds. I am hopeful that I have found a potential missing piece of the puzzle to explore.
I wish you well TB.
Dr. Russ
Just wondering if there could be a connection between epilepsy and scar tissue. If scar tissue prevents nerves from sending messages to other parts of the body, and the epilepsy is unexplained, could it make sense that scar tissue from a neck or head injury could create the disruption in the signal? My son has been on epilepsy medication since he was 14; seizures hit out of the blue, however he injured his back the year before the seizures started, and then a few months prior to the seizures starting, he had a bad tumble from a motorized scooter (not moped type scooter). Mothers! We’re always looking for explanations or a fix 🙂
I’m glad I found your website; it’s informative on many levels!
Great question Lynne,
By the way, you would probably appreciate the blog post I put up today over at my Doctor Schierling dot com site. I have an article I wrote about the fact that much epilepsy is now recognized as autoimmune. Although head injuries are a definite potential cause, I have not heard about back injuries — particularly a lower back injury causing epilepsy. It would not surprise me, however.
Sincerely,
Dr. Russ
Dr. Russ,
Thank you for the response! Interestingly enough, autoimmune diseases run in the family, so I’m definitely checking out your new blog.
Peace,
Lynne
Hope you find it helpful.
Russ
Hi,
I just started using a piece of equipment for my cellulite and I have these fascial bruises on my thighs, any idea how long before they are gone? Also, should I continue to use this piece of equipment while the bruising is still present?
Thanks
M
My first question is what sort of equipment are you using?
Dr. Russ
Fasciablaster probably!
Love your article!
Hello Christy,
I had never seen that creature til I looked it up after your comment. Interesting. Thanks for the comment.
Dr. Russ
Great, clear and informative. Finally
This is the most awesome article I’ve read! I have been told u have tissue connective disease, fibromyalgia, Sjogrens, lupus, osteoarthritis, sleep apnea, bone spurs, disc disease, etc. I’m researching & feel I’m fighting for my life. I have some decent doctors but they even admit they don’t understand all that I have going on. All I have it a lot of hellish pain, & fatigue. I want the right answers for the right help. Thank u for this info & I’d love to know more.
Peace
Hello Julie,
If you really want to know what it’s going to take to solve this problem, make sure to visit my blog and type the word “EXIT” into the search bar. It will show you how to create a personalized Exit Strategy for chronic illness, inflammation, autoimmunity, and pain.
Thanks for the props. Glad I am able to make a difference.
Dr. Russ
I recently broke my tibia and fibula in a sporting accident. After the operation where an intramedular rod was inserted in the tibia I got compartment syndrome. They cut open the fascia in my lower leg in both sides. As a result I have very poor range of motion in my foot. I was wondering how I could get this range of motion back? Massage and working out? I was also wondering if fascia does grow back!
Hello Linus,
I can tell you from experience that the Tissue Remodeling I do does not work well on compartment syndrome of the lower extremity (not much experience with the upper extremity). Post-surgical therapy is critical with this sort of thing. As to whether or not Fascia grows back, it can certainly heal, although it will tend to have restriction in it. Massage might be beneficial, and can’t really make anything worse.
Sincerely,
Dr. Russ
Hello thank you for the information which you are sharing!I have question if you could explain- Im weightlifter and my left Ql+iliocostalis lumborus +erector spinae are overdeveloped than right.I had painful spasm when i tried to stretch left erector and when i touched more deeply my musculature in the left side the muscles are very solid and i feel how the erector is pulled more to left side i have functional scoliosis also left leg is with lower ilium.The muscle-iliocostalis is skipping when i massage it with ball but it hurts a lot and the pain is starting to spread in whole ilium front and back.Is this overstretched fascia, knots ?Can i use collagen injection therapy?I have started to train my right side and the pain in left don’t show up but if i train both sides i feel it.I don’t do massages with ball just training weak side but i feel the muscle on left don’t allow maximum hypertrophy on right.
Thanks
Hello Ira,
There are two major reasons this could be going on — either purely neurological, purely, mechanical (subluxation, scar tissue, scoliosis, short leg, etc, etc), or a combination of both. My site is loaded with information that pertains to addressing all three. As to the collagen injections you are wondering about; I don’t have any idea.
Sincerely,
Dr. Russ
Does the lymphatic system have anything to do with fascia? Also I think injuries have accumulated in my left rib area. I’m not sure if it started as a hernia a few years after a right mastectomy. I developed cramp like symptoms when doing sit ups. Then 10 years later second mastectomy. Now pretty much constant swelling and pain on left side 5 years after surgery, radiotherapy. When I push against it, pains alleviated when it feels like it’s cramping. I am overweight but was not as big when it first occurred. I see a lymphodema nurse and she wants to treat it with a machine that lifts and stretches. She’s currently treating me for cording/shoulder pain round left arm. Which has worked so far, releasing my hand and neck. Anyway really interested because my husband has complex regional pain disorder, so I now think my nurses machine could help him too! It has certainly helped me! email
Lymphatics and Fascia are ubiquitous in the body, and very much related to each other. Not an expert in lymphedema, not sure what sort of machine this is.
Dr. Russ
What interesting information! I was wondering, are fascial adhesions noticeable? I injured my ankle years ago and, shortly after, a large grape-sized bump grew on the arch of my foot. My family doctor took an x-ray and, when nothing of interest showed up in the x-ray, she waved away my concerns. I did my best to ignore the pain and hoped it would heal itself somehow, but that didn’t happen. Recently, I went to a foot doctor who stuck a needle in the mass, thinking that fluid needed to be drained, but there ended up not being any fluid. So then I got an MRI done of the area, only to be told that everything looked fine. Talk about confusing! Here I am with a noticeable bump on the arch of my foot, yet the MRI shows noting out of the ordinary. Could I have a fascial adhesion there? Do you know of any doctors in the Detroit area who perform your tissue remodeling treatment? Thank you.
Hello Mrs. Writer,
I seriously doubt that your problem is a Fascial Adhesion. It’s probably more like a callous, but without looking it’s tough to tell.
Sincerely,
Dr. Russ
I took the fluoroquinolone antibiotic Cipro all the way back in 2009 and have been completely crippled ever since. Twelve pills was all it took. My fascia literally disintegrates all over my body for no apparent reason whatsoever, causing me to be completely bedridden & in suicide-level pain. I’m barely able to stand up anymore, as my joints can no longer bear my own weight. Doctors do not even attempt to help me. The vast majority have even scoffed at the idea that Cipro could have even done this to me. Their ignorance has cost me my life. Fluoroquinolone antibiotics (I know NOW) attack collagen, causing spontaneous tendon ruptures, chronic ‘tendonitis’ that doesn’t go away, skin sagging, retinal tears, neuropathy, fasciitis, etc. I was only 30 years old when I was poisoned by that drug. Everything I had that constituted a life is now long gone. I was forced to move back in with my parents and collect SSDI now. I am EXHAUSTED from fighting this battle and cannot wait for it to be over. It appears that death is the only way out of this. Please be aware that Cipro, Levaquin, Avelox and ALL other fluoroquinolone antibiotics are detrimental to your connective tissues. I wish someone had warned me.
Hello J.
I have a number of posts on Antibiotics in general, and Fluoroquinolones specifically, over at my Doctor Schierling dot com site (all on the blog). In fact, I am almost positive I have a link to your site. Because, as you say, doctors don’t think these drugs do this to people, you and others like you are never counted as a statistic. Thus, the side-effect profile for extremely dangerous drugs like Levoflaxin or Ciproflaxin looks far better than it really is. It breaks my heart to see the numbers of people dealing with this nightmare, who are being totally ignored by the medical community.
Sincerely,
Dr. Russ
I too took cipro for a week and was so sick the whites of my eyes became inflamed and it was excruciating to blink. I have tendon issues and fascia stiffness and neuropathy if both legs from calves down. I’m so sorry to hear about your outcome. After reading your comment it makes sense to me why I can’t run anymore and I’m in so much pain also had 2 tendons -pereoneal a worked on and I still can’t walk 1/4 of a mile without limping and exhausting pain or fatigue. My Achilles’ tendon has contracted and won’t bend my ankle up and more than 90 degrees. So dorsiflexion inhibits my walking. Even after gastric recession it just won’t budge. My prayers go out to you. Thank you DrRussell for you informative posts.
The problems associated with fluoroquinalone antibiotics are not only brutal, but ridiculously under-reported. I would beg people not to touch this class of drug with a ten foot pole. If it’s going to hit you like this, it happens the very first time you take them — no warning.
Sincerely,
Dr. Russ
I have had the fascia removed in my left lower leg from the muscle somewhere between my rib and rib. I am in excruciating pain and have uncontrollable muscle spasms and cramping. Is there any possible way to fix this issue? I’m feeling that amputation is the only cute at this point. Need to mention I have extensive tendon issues too.
Thank you, Tina
Not knowing exactly why you had Fascia removed from your leg and rib makes figuring out what is going on almost impossible. Make sure you read my articles on Systemic Fascial Adhesions and Systemic Tendinosis over at my Doctor Schierling dot com website.
Sincerely,
Dr. Russ
Very fascinating and well-written article; makes a lot of sense!! Thank you.
I’ve been practising martial arts for over 5 years but my body is not flexible (especially the right hamstring).If I do some prolonged jogging and warm up, I will eventually approach full stretch ( e.g splits)but after some hours I get sore at the centre of my femur (middle part of attachment of bicep femoris) .I very much suspect myofascial adhesion.
Hello Wale,
You probably just diagnosed yourself. I am, however, aware of individuals (a good friend who is a martial artist) who, despite their constant stretching, are just not very flexible.
sincerely,
Dr. Russ
You have so much amazing information on this site, I couldn’t be more grateful to you for sharing it with us!
I’m a tennis player that developed a repetitive strain injury eight months ago around my right elbow; I had burning sensations, coupled with periods where the entire arm felt ice-cold, and was “diagnosed” with both tennis-elbow and ulnar-nerve dysfunction, though neither through tests or extensive examination.
Eight months on, I still can’t bend the elbow without pain or a feeling of restriction; I can’t wear anything with sleeves because it irritates the whole area around the elbow.; when I sleep I have to build a bridge with pillows so that the elbow isn’t touched by anything. The “pain” feels similar to the burning/irritation you would get when you scrape your skin, only far worse. There is swelling on both the inner and outer-sides of my elbow/arm.
Do these symptoms match fascial adhesions?
Thank you!
Best guess is that this is nerve-related and not a tissue issue (although it might very well have a tissue component).
Sincerely,
Russ
Hi, I have reflex sympathetic dystrophy in my right knee lower leg. what you describe sounds a lot like what I have. I have very sensitive skin and quite often can’t stand anything touching it my husband took water pipes and put them together and I lay a blanket over top of it to be able to keep warm at night or I can’t stand anything touching it I describe mine as filling as if you hit your funny bone at your elbow but that feeling doesn’t go away and I think it’s worse than a burning pain I get at times it makes it extremely difficult to walk and because of the risks risks involved I can’t have my knee replacement this happened after my third surgery on my knee. I apologize for all of the misspelled words and The errors. I am having difficulty with my fingers today so I’m using the recording and it at times is incorrect.
Hello,
I am scouring the Internet for answers as I have been dealing with chronic pain for five years now. I can’t tell you how many doctors/specialists/chiropractors/osteopaths, etc I have seen, all I know is that I am now in debt and still in pain (low back pain, right side).
I was initially diagnosed with a locked SI joint which was still painful even when the physiotherapist got it somewhat stable. I had four rounds of prolotherapy injections, which got my SI joint nice and stable but the pain was still there. I’ve now been told the source of pain is coming from my lumbar spine (L5 S1) and had a spinal block last month to “freeze” the nerves. Most people respond very well and are pain free within minutes. It didn’t relieve one bit of my pain. The specialist wondered if it might be the muscles that are causing me such pain. The area is very sensitive, in fact, sometimes it feels like the skin in the L5 S1 area is itching or burning. Very strange. The specialist suggested deep tissue massage, and I’ve had three so far, with no pain relief whatsoever.
I have fallen into a depression that I can’t shake. I used to be a runner, so energetic and loved being active. No one seems to have any answers for me.
I can tell you that both PS or Fascial Adhesions of that area are often associated with SI dysfunction and pain.
Sincerely,
Dr. Russ
Hi there. Great website but I am stumped. I wonder if you could shed insight?
I am 32 years old, athletic, and for as long as I can remember I have never been able to “lock” my knees and touch my toes. Trainers always tell me it is a flexibility problem and I should stretch more.
The problem is, when I stretch (either / both knees locked, and leaning forward towards toes) I get an intense, almost system-wide pain that seems to radiate from behind my knees. I can’t describe it well. It’s not like any other pain I’ve felt. But I can feel the pain in the pit of my stomach, and it is impossible for me to push through it. If I did, I almost feel like I would have to go to the bathroom.
Went to a few trainers, a chiropractor (who suggested it might be tight fascia) but no luck finding treatment.
Thanks.
Thanks for the compliment Brett,
Although it was written especially for people with Piriformis Syndrome, THIS ARTICLE on overstretching might be right up your alley.
Sincerely,
Dr. Russ
Hi Dr. Russel Schierling.
I’m a medical student with a chronic pain problem in my arches/heels (bilateral).
I have no pain during the first steps in the morning, nor when stretching the arches. My pain is worst when STANDING STILL. It will exponentially get worse the longer I stand completely still and it will get better INSTANTLY as soon as move out of place (start walking). I will not have pain while walking until hours into my walk, but only minutes if standing still.
Doctors have tried most standard plantar fasciitis treatments and nothing has worked. I’m currently doing a very rigorous stretch program but I’m not seeing any results.
What are your thoughts?
Regards, Bjarni J.
Hello Bjarni,
As crazy as it may seem, this problem could be coming from your back.
Sincerely,
Dr. Russ
Thank you for your reply. You’re referring to the superficial back-muscle line? I’ve read a bit about it but I’m unsure how to proceed and I doubt I can find a physician in my location that has read anything about it.
Can you guide me on a next step? Any exercises I can do that you know of?
Actually, nerve irritation caused by VERTEBRAL SUBLUXATION can cause a wide array of strange and seemingly unrelated symptoms. Not saying this is what it is, but it could be. Do you have chiros or osteopaths in your area who could evaluate you?
I had Ultherapy on face, cooked me to 160 degrees. All dehydrated fascia on face, immobile forehead, tight eyes. Would this work on face? Any tips?
Hello Tara,
I do lots and lots of work on the head (face / skull) as you can see if you take a look at my Doctor Schierling dot com site. However, I must say that I have never treated anyone with this before, which makes it almost impossible to answer your question accurately.
Sincerely,
Dr. Russ
I have pain in my arms that was diagnosed as tendinitis, even though I have no pain specifically in my elbows, just weakness in one inner arm muscle and cramping in the other. I have had a range of symptoms as this has progressed going on over a month now. At first it was tightness in the forearms. I had a massage and the massage therapist said something about the fascia but I didn’t really understand what it was. Then I started having cutting/burning pain in the backs of my thumbs, index and middle fingers of both hands. I also noticed that my veins looked engorged. PCP gave me raised eyebrows, and anti- inflammatories, and subsequently oral steroids (Medrol dosepack). That made the stinging in my hands go away at least! I have a sit down computer job. I still have pain in the muscles with use (inner arm), and I am unsure if this could be due to adhesions? I also have pain leaning on the inside of my wrists (not on the palm), like where your veins run. Is this what you treat?
Hello Christen,
This sounds like you might have a systemic tendinosis. Look back through the comments, as I have provided several links on this (you may have to look at comments under Tendinosis).
Sincerely,
Dr.Russ
I believe I have torn the Fascia in my belly region, as I woke one day to find a bulge there. I “feel” movement there and even experienced a flushing symptom that made me feel like I was going to faint while I was driving. I have seen several doctors and gone to the ER several times trying to get someone to listen to me…I only hear that “this is your body, get use to it”. I believe the bulge is getting bigger and it has really affected my physical athletic lifestyle…I finally got a sonogram and was told there was definitely something there…I feel it is my muscle and organs pushing thru. Am I destined to have this bulge the rest of my life? I haven’t found anyone else who has this condition around their belly region.
Very tough to say, but Diastasis are common. If there really is some sort of tear with things pushing through, this would qualify as a surgical problem.
Sincerely,
Dr. Russ
The cause of my severe chronic pain was explained to me by a specialist. He said the facia in my lower legs is 3 times the normal thickness & looks like it didn’t grow properly. He thought it was a birth defect where I have not enough elastin in my fascia & too much elastin in my joints (I am also hyper mobile). I have been in pain with this for 36 years now & still no one has given me more than 6 months slight relief. Please can you tell me if you’ve ever heard of anything like this? As all my specialists are confused & scared to do anything (I have asked for bilateral amputation but they refuse), do you think ultrasound may help break down the scar tissue from my previous operations?
Wow Manda,
I have never seen anything like this before. Not sure what might help you, but ultrasound for your problem would probably provide no benefit.
Sincerely,
Dr. Russ
I tore the muscle and fascia in my lateral oblique abdominal muscle as a result of a severe fall 4 months ago into the corner of an immovable wood burning stove (not currently in use). I have been to multiple doctors of no help and am currently working with a PT who is trying to somehow manipulate multiple adhesions which are causing pain in my left torso and the left part of my middle back. Is it possible that new adhesions are forming, “fixing” multiple organs in place and causing increasing pain?
Hello Diane,
This is not an injury that will cause adhesion to your organs, although it could certainly feel like that’s what’s happening.
Dr. Russ
First let me say that I am impressed that you answer. I have chronic back pain. I have 5 bulging discs, spinal stenosis, facet joint disease, sciatica, arthritis and now my dr possibly thinks the fascia in my back is deteriorating. The reason is that just touching my back feels like I have been beaten with a bat! It is miserable. My job is riding 40 hrs a week on a school bus for the last 28 yrs. Does this sound like the fascia is bad? How do I know if an MRI doesn’t show it?
Oh yeah one more thing…I had a massage done on Mother’s Day and I couldn’t walk out of the building for an hr. When I got home I had to crawl up my 9 steps to get into the house and literally could barely walk for 2 weeks! That’s the last massage for me! Every muscle in my back flipped out and it was so tight that I couldn’t function. Looking forward to seeing your reply.
Hello Sheri,
With all that going on, your Fascia definitely has issues. However, you need to start dealing with the underlying inflammation before you do anything else. I have tons of articles on my blog.
Sincerely,
Dr. Russ
My husband is 64 and recently woke up to discover a buldge on his left lower side. After 4 Trips to the Er where they kept saying this is just your body, and one event where he almost passed out while driving, we finally found a doctor who would listen to our theory that he has torn his fascia and his muscles are protruding out. Finally a sonogram confirmed a mass in the area. He tapes it up during sports, wears a belly band, but he feels like his quality of life has dimenished because of this condition. In all the articles we have read, there is no info on any repair of this to push the muscles back in! Do you know of such a surgery? What’s it called? Thanks, Cathy
Hello Cathy,
Not sure what it is called, or if that is what it is. This is something that doctors should be able to tell you — but I am not surprised that they can’t.
Sincerely,
Dr. Russ
thanks for your reply, yes, we have seen several doctors and 2 specialists and no one has an answer for this problem. He has a 5 inch by 3 inch protrusion on the left side of his body between his navel and his side…and it is definitely not suppose to be there, yet it is not a hernia. It is fluid feeling and interrupts his sports as it gets sore easily and larger after sports..he wears a belly band to hold it firmly in…a sports doctor he sees massages it and that really doesn’t seem to do anything at all. An internal surgeon heard his story last week and said he had no idea what it was. There is nothing out there on the internet similar to it…It is not diastasis.
Hello Bill,
Wish I could be of more help, but not sure — does not sound like a Fascial Adhesion issue. Let me know what you find out as it always helps me with similar patients.
Sincerely,
Dr. Russ
Thank you for this excellent article! I have been undergoing scar tissue remodeling here in Canada with my own Chiropractor on my knee that I cracked back in the winter. It has reduced my pain and improved my ROM tremendously. I didn’t understand the importance of doing the prescribed stretches until I read your article-Thank you!!
You are welcome Sarah.
Dr. Russ
I have chronic mid back pain my muscles. Now I guess IF I am understanding correctly it could be the Fascia that is what’s hurting me. All I know is I need help! I do not understand the treatment that is involved.
There are any number of treatment approaches to breaking up Adhesed Fascia. Lots of info on my DoctorSchierling dot com site.
Sincerely,
Dr. Russ
Hi Doctor,
I am 28 years old, male. I had pain due to Ulnar nerve compression in left elbow, for which I underwent an Ulnar nerve transposition surgery 6 months back. However, I feel pain in the elbow region around the ulnar nerve, especially with my left elbow lying on the bed in the resting position. My surgeon feels that this could be because the ulnar nerve could be having an adhesion with the surrounding scar tissue that may have been formed around the nerve after the surgery. Please tell me how to treat it. Thanks.
Hello Madhur,
I actually see a great number of people who have issues with this surgery. Find someone good at breaking the tissue up (you might be able to do it yourself). However, start easy because you don’t want to damage that potentially entrapped nerve.
Sincerely,
Dr. Russ
I tore my quad muscle and heard a pop. It’s been 3 months since it happened. I’m not exercising and walking without pain, but I still have a lump where my Quad tore? Will the lump in my leg ever go away? If so, when? Thanks so much. I’m reluctant to play any sports where I may re-injure my leg.
It may never go away, but with proper treatment, the Scar can be made more functional. Re-injury is always an issue — particularly when you start using it after injury.
sincerely,
Dr. Russ
I have had an MRI, xray, PT and seen my PCP and Physiarist and the latter thinks it is fascia. I have stiffness rising from seated position and if I stand or walk more than ten minutes a tightness grows from my psis area to my midline l5s1. I then simply sit or stretch forward and it “resets” and I can continue. Some daysi get only five minutes and occasionally I get up top 15. I see a sports med person in two weeks. Does that sound like facia? I was extremely active when this started and was walking up to ten miles a day. For the first year I had it, it would go away for a month or two at a time and then return for a week or so. But now I’ve had it since the beginning of April continuously.
Head on over to my doctorschierling site and check out the article I wrote called “Chronic Low Back Pain and the Thoracolumbar Fascia”.
sincerely,
Dr. Russ
Hi doctor schierling, my name is tony I had a spinal fusion 6 months ago I’ve been feeling this knot,marbles, brick feeling in my back .i do have hardware in my back .. Could it be the hardware or scar tissue??
Hello Tony,
It should be fairly easy to tell the difference. If you can roll it around, it’s definitely not the hardware. If it’s too deep to lay a hand on it, your guess is as good as mine.
Sincerely,
Dr. Russ
Hi Dr. Schierling,
My name is Emily,and I have been dealing with constant everyday 24/7 pain for the last 5 years. All the test come back showing nothing. Some of my doctors that I see,think that laparoscopic would be the way to go,to be able to take a look inside to see what is causing my pain,but the surgeons won’t do it. My organs are fine,and there are no masses,and no hernias. So my question to you is if I had fascial adhesions,would a laparoscopy show the fascial adhesions? If so,could they be repaired surgically while the surgeon would already be in there? I seen in this post that you said that you can take care of fascial adhesions through I.I.R.E.C.B.C.T “Tissue Remodeling” ? I have this bulginess in my upper left abdominal muscle area. It feels like my abdominal muscle is being pushed up into my sternum area and over onto my left ribcage. My left back muscle is always tensed up. My left side of my ribcage hurts,and feels pushed out a little bit. I have muscle spasms on both sides of my upper abdominal muscles,and on my left side and left side of my back. Sitting upright applies pressure to that bulgy area,and amps up the pain even more,also physical activity amps my pain up as well. When I go turn my body it feels like my muscle is being restricted causing alot of pain. Reclining in a chair or lying down are the only things that bring the level of pain down. I’m just so miserable all the time,and so frustrated cause so far,no surgeon will go in laparoscopically to look for the problem since the test aren’t showing anything. I was on pain meds for the first 3 years,tried muscle relaxers,anti-inflammatory medicines, steroid injections,intercostal nerve block,and physical therapy,and a chiropractor,but couldn’t remain seeing the chiropractor for very long because of my insurance. Up to this point nothing has worked. I just need to get whatever wrong fixed,so that I could know what it’s like to be pain free again. I’m trying work and take care of my 6 year old daughter,and with this pain it makes everything very hard to do and is very challenging. Would you have any suggestions of what I could do to get to the bottom of this agonizing constant pain? Your advice would be very appreciated!
Sincerely,
Emily
Hello Emily,
The laproscopy will show fibroids and / or adhesions, but not Fascial Adhesions. Email me some contact information, using my contact page on my Doctor Schierling dot com site.
sincerely,
Dr. Russ
I had a lot of these same issues. My pain went from my feet all the way up my legs, through my pelvis and into my entire back, neck, and face muscles. I spend two+ years and thousands of dollars seeing different therapists: two chiropractors, a fascial stretch therapist, three or four massage therapists, a craniosacral physiotherapist, and I’m probably forgetting a few others. I finally found relief with a PT trained by the Postural Restoration Institute. PRI uses breathing while activating certain muscles or groups of muscles to free up the fascia that’s stuck and impeding proper movement mechanics. Your PRI therapist will likely give you a bag of balloons and a small ball to work with. They seem very simple, as do the exercises, but my god, these have been a life saver! PRI took me from a 9 or 10 out of 10 in pain to about a 2 or 3 at it’s worst. Here’s an example of the PRI exercise that has helped me the most so far: https://www.youtube.com/watch?v=4GoqjoEXaAw
Thanks Ian,
I look forward to learning more about this. I have always said that there is a solution out there for everyone; it’s just a matter of finding it.
Dr. Russ
Hello Dr. Schierling,
Due to excessive sitting under stress for prolonged periods for several years and a lack of exercise, I developed lots of muscle tightness in my core, upper legs, and pelvic floor. I have been seeing a physical therapist and undergoing deep tissue massages, both of which have helped quite a bit.
My therapist and I have noticed that I seem to have lots of dense, sensitive fascia in my groin, in the area above the genitals but below the abdomen. While massaging this area, I feel soreness in my pelvic floor and one of the muscles in my pelvic floor will spasm continually.
Do you have experience remodeling the fascia in the groin/pelvic floor area?
Thanks!
Brad
Hello Brad,
Tons of work on the groin. Pelvic floor is definitely its own specialty. My Doctor Schierling site has an article on Fascial Densification.
Dr. Russ
wow! everything above relates to me. I think i finally have a answer to my chronic pain? i have cecs, i had a fasciotomy last year which did not help. ive been told i have fibromyalgia and every other kinda condition under the sun. My Gp doesnt take me seriously maybe thinks I’m just a drug seeker? I’ve recently got pain all over my back. and i never realised theres fascia there too. the Cecs is in my lower legs and now I’m pretty sure m legs and back are linked. Thank you doctor 😀
Hello Yvonne,
Your back and legs are linked. Make sure to go to my Doctor Schierling site and read my article called, “CHRONIC LOW BACK PAIN AND THE THORACOLUMBAR FASCIA”. Wish I could tell you I have had good luck with Compartment Syndrome, but unfortunately, I have not.
Sincerely,
Dr. Russ
Great site, very informative.. I am 57, female. Over a year ago,had butt pain that generated throughout my left leg. MRI showed bulging on l2 , l3, l4, l5 and S1, with nerve root compression on left. and slippage on l5/S1. Prior history in last 20 yrs includes a fall while skating on buttocks , re-injury to buttock while sliding out a tunnel above the water in a water park, a fall at a grocery store, where left leg/buttock affected (recent in 6 yrs), left knee pain that shots temp fixed. have done PT, had several shots in spine to ease nerve pain in leg, had treatment for inflammation, etc. continue to see pain doc. do not take muscle relaxer or pain meds unless cannot sleep, or tolerate pain. now back pain is prevalent, with occasional leg pain. butt pain is there when mostly sitting, walking too mush, standing too log, bending, lifting, etc, disability denied, but in appeal. i work with limitations and rest in between. is ps possible here? If I were your mom/family member what would you recommend for me? I do not like taking meds, makes me sleepy, groggy, dizzy, and dry mouth. I am thinking about putting in a pool to eliminate the back issues and allow me to exercise,even though I cannot really afford it right now. I cannot ride my bike anymore, dance like I used to,walk long,etc. i want to be positive and keep moving, but afraid that it is making it worse.
Hello Eileen,
It’s interesting that you brought it up, but I try and make all recommendations as though they were to my mom, dad, family, etc. This is the sort of problem people come to me wanting Spinal Decompression for. In cases like this (due to “Asymptomatic Disc Herniations” — see my Doctor Schierling site) I will typically try a Tissue Remodeling treatment just to see if the problem might be PS. Make sure to look up my Piriformis Test on my Doctor Schierling site as well.
Sincerely,
Dr. Russ
Hello Dr. Schierling,
My name is Abigail, I’m 19 years old and have been dealing with shoulder, shoulder blade and rib pain on the right side of my body for 3 years. I’ve had two MRIs, one with a dye injection, and I’ve visited 2 different doctors. One said he saw a cyst on my shoulder blade and prescribed 800mg of Ibuprofen twice a day. I did that off and on for 1 1/2 years. It helped with the pain a lot at first. Almost made it go completely away. But after a while I started feeling the pain again. I started to think the Ibuprofen wasn’t doing anything until I stopped taking it and the pain was so much worse. I finished the prescribed amount of Ibuprofen, and still take two 200mg when the pain is really bad, but it doesn’t help much. Another doctor said he thought it was a labral tear, but the MRI came back clear, so he just suggested physical therapy. I have lost some mobility in my shoulder. It pops sometimes which makes the pain worse. It feels almost like a pulling, sharp, aching pain all over the upper right side of my back, into my right shoulder, and the right side of my neck. I also have pain in my right rib cage. I’ve been told it is a problem with my fascia by a massage therapist I visited. She suggested Myofascial Release therapy. Another massage therapist suggested something similar. I’ve done some research, and I’m not sure if either of the treatments will help. Some articles say they are experimental which makes me nervous.
It’s been a long 3 years with this pain. I don’t even remember what it feels like to be pain free. Can you give me any advice? Does it sound like a fascia problem to you? Do you think Myofascial Release Therapy will fix the problem so I can be pain free?
Thanks in advance!
Abigail
Hello Abigail,
Have you seen my bruising page? If your massage is not relatively harsh and uncomfortable, it probably is not getting deep enough. Tons of information on this on my Doctor Schierling site. BTW, you will ruin your kidneys and liver doing that much medicine. You have to find a way to get off of it.
Sincerely,
Dr. Russ
Hello Dr. Russ,
I have limited flexibility and stiffening in my lower back, pelvis area and between my thighs with tightening of the hamstrings, due to a Spondylolisthesis (forward displacement of the fifth lumbar vertebra). I guess this is because the fascia is excessively contracting itself to support my injured lower back, trying to protect the affected area. Isn’t it?
Perhaps removing or cutting surgically some of the fascia in this area could help me loosing up a bit around my inner thighs and increase my flexibility around the legs and lower back area?
Sincerely,
Arnaud
Hello Arnaud,
This might sound good at the time, but remember that the area will heal with Scar Tissue. Also remember that a huge number of people are walking around with grade 1 or 2 spondylo’s. My best guess is that these two things might be related less than you think.
Sincerely,
Dr. Russ
Dr Russ, Please can you tell me would ultrasound be able to see tears to the fascia under the scalp and thoracic area of the back , are there any scans that can see serious damage to the fascia
Hello Sue,
Go to my Doctor Schierling dot com site and take a look at my post on “Imaging Fascia”.
Sincerely,
Dr. Russ
I read your article about fascial adhesions and I have some questions regarding adhesion pain. I had chronic exertional compartment syndrome in both lower legs and I had all compartments released during surgery. I am about a year and a half out of surgery and still am competing competively in athletics. There is a spot under one of my scars on my leg that hurts mostly to touch but is bothered sometimes by running. I had ankle reconstruction this past January and so I have not been running really since that but now that I’ve continued activity, it is bothersome and continues to bug me more and more. I’m so tired of injuries and sitting out and am just curious if it could be fascial adhesions due to the fasciotomies or a bundle of stitches, or scar tissue or what….and what is my best method to go about figuring out what it is? Thanks for your help!
-Liz
Hello Liz,
Firstly,
I have worked on people with CS of the lower leg and not been able to change it. I have been able to help a lot of people who have Fascial Adhesions due to any number of different kinds of surgeries. As to how I know if the problem is due to Fascial Adhesions — I just treat it and see how it responds. This is because Fascia does not image well on MRI — the standard test used to look at these problems if they become ongoing.
Dr. Russ
hi Dr. Schierling, thanks for this helpful article. four months ago I had a nasty fall, landed on my butt on the edge of a step. HUGE black bruise covered one buttock, with lots of pain and swelling. When the bruise finally faded I still had a big lump, which I assumed was a hematoma. Now what’s left is an egg-sized lump, which shows through my clothes. I was devastated this week, I finally went to have it surgically removed and found out it’s not a hematoma, not blood-filled. the doc said it’s an adhesion or scar tissue, which forces the “normal” fatty tissue above it to protrude like a muffin-top. My insurance won’t cover ANYTHING so whatever I do is out-of-pocket. I’m in the Seattle area, do you have any suggestions? I’m a yoga teacher, so this is really a bummer! thanks, Diane
Hello Diane,
Firstly, if you are concerned about the cosmetics of this Scar Tissue, the only thing that is physically going to “remove” it is surgery. However, some intense body work will likely make it more functional and give you fewer problems over the long haul (HERE).
Sincerely,
Dr. Russ
Hello Dr. Russ,
I am a 19-year old college runner (cross country/track) who hasn’t been able to compete at all in my first 2 years of college because of various injuries. My more recent ones have all occurred in my right proximal quad. In the winter of 2013 I “strained” (Doctor’s word for it) it with low mileage just getting back into running after a tibial stress fracture, and with physical therapy it was fine within 4 months. But this past September a similar injury occurred in the same spot after running for 6 miles up a mountain (I should’ve seen it coming), but far worse than before. It is now 9 months later and though I don’t feel the same pain as my original injury, I feel pain in my quad whenever I lift my leg with my knees locked or extend my hip on my right side . Going into a lunge is painful. Running for any amount of time, and even sometimes walking hurt. Also when I lift my right leg, I can see that there is an area where one of my quad muscles is more clearly delineated under my skin than it is in my left side, as if there is a more defined border between it and the adjacent muscles. In that area I can feel tangled bumps under the skin that move around a little if I rub them. The little bumps run all the way from the interior side of my knee up to where my quads meet my groin, though the biggest ones are in one spot in my upper thigh. Could these be facial adhesions? I’ve had several x rays/MRI’s the last couple of years that have shown healthy bones and muscles despite my pain. I have been doing a lot of quad/hip flexor stretches as well as foam rolling but to no avail.
Thank you,
Sarah
Hello Sarah,
The very first thing I would do is head over to my DoctorSchierling.com site and pull up my blog category on “Inflammation” and start reading. Best guess (and that’s what it is) is that you have a combination of Hip Flexor Tendinosis (I have a page on this) as well as some serious Fascial Adhesions of your quadriceps. Did you ever struggle with Osgood Schlatter?
Dr. Russ
Hi Dr. Russ,
Thank you so much or your reply. And also, both for your blog post about inflammation and just in general the work that you do; it helps so much just to be able to what’s going on with my own body a bit better.
I’ve never been diagnosed with Osgood Schlatter but when I was a freshman in high school, I did have runner’s knee, though I don’t remember which side. It cleared up with PT and hip flexor exersices.
Thanks again,
Sarah
My son has been suffering g from what doctors thought was planter fasciitis and/or possibly some sort of rheumatoid arthritis. This came on very quickly in one foot the weeks later in the other. He had to stop playing hockey and baseball. It has affected all of our lives dramatically because it’s a factor when planning family out tongs, vacations and even looking for colleges. The pain is always there for him. There was no known injury. He wore the boot, orthotics, heel pads and night splints. He did shock wave therapy and Accupuncture which were both painful. He tried arthritis medications as well. Nothing has dulled the ache in either foot not even a small bit.
I want him to be able to walk without pain and do what he loves to do. He’s leaving for college I the fall. He has a zlion MRI’s and some say planter fasciitis and the doctors at the Hospital for Special Surgery in NYC say their radiologists don’t see that.
Can you help him?
Karen
Hello Karen,
Take a look at the article I wrote the other day for my DoctorSchierling.com site (Tell Me Again Why You Want an MRI?). The two problems — RA and PF are totally unrelated — except for the fact they are both inflammatory. Make sure to look at the same site because I have information on both. For starters, I would probably do an Elimination Diet to figure out what foods he is sensitive to (if any). If addressing this along with Gut Health doesn’t help, I would at least talk to Shawn over at Xtreme Footwerks in Idaho Springs, CO. Doubtful I would be able to help you with this.
When you get this problem solved / figured out, please drop me a line and fill me in.
Sincerely,
Dr. Russ
hello
I live in Michigan and fear I am so afflicted with this I am dying a slow painful death. I have seen so many doctors Who claim to know whats best for me I could just scream. I have fired them…begged..cried…you cant imagine. Now i am reading your website and find what i feel is my only hope. Could you please tell me if there are other doctors out there in my area who can do this? If not I guess my goal will be to move to where you are. Please save me
Laura
Hello Laura,
There are any number of practitioners in every state doing similar things, although I don’t know anyone doing quite what I do. Sorry, but I don’t know anyone in your neck of the woods.
Dr. Russ
Dr. Russ,
At 57, I’ve been told I should no longer be riding horses, and up until 2 weeks ago, I would have vehemently disagreed. However, I was injured when my horse panicked under a bridge and I wound up with severe trauma to my right pelvis area. The pain is excruciating! My doctor has seen me twice for remolding, and the last time the pain had me just screaming. What would be appropriate management, as right now I am worsening. There is burning pain and severe swelling at the initial injury sight, and to be honest, I’m hesitant about going back after the last session. The procedure left me in tears and I don’t normally cry. Help!
Hello Linda,
I’m a fan of horseback riding and have always said that it’s therapeutic until something goes wrong. As for the remodeling, I never remodel an area that is “severely” swollen. It’s difficult for me to give you any meaningful advice not really knowing what your doctor has done.
Sncerely,
Dr. Russ
Hi there. I received a blow to the side of my knee a few weeks ago while playing sport. My GP said there was no major damage and it was probably a fascial injury. He just prescribed anti-inflammatories. When I apply light pressure at the medial side of my patella, I get a pain shooting right across the front of my knee to the distal side. This does tie in with your article and I wondered if remodelling is appropriate (also would need to find a practicitoner in Australia)
Hello Clare,
The doctor could very well be correct in his assessment that the injury is on the outside of the knee (the Fascia) as opposed to the inside (Ligaments, Cartilage, Bone, etc). The thing to remember is this; most medical interventions (including NSAIDS and Corticosteroid Injections) are exceedingly harsh on multiple body systems. And while Tissue Remodeling might look harsh due to the bruising, it’s worth a try as you can’t really make things worse. In other words, there’s a tremendous upside, with no real downside.
Sincerely,
Dr. Russ
Hello Dr. Russ.
I have had heal pain for 10 months now and have tried physical therapy, cortisone shots, acupuncture, massage therapy, osteopathic manipulation, herbs, poultices etc. The most recent doctor told me I have a heel spur and significant tear in my facia with a thickness of #7+. He suggested a surgical procedure with AMNion injection. Can you please weigh in on this. I’m tired of the pain I can barely walk and need to do something.
With gratitude,
Julie
Hello Julie,
Plantar Fasciitis is one thing, but when you start talking about tears in the Fascia, that’s something altogether different. I know they are using Stem Cells for joint problems. The thing is, the PF is not a joint. Simply go to PubMed and look up the studies; then start going around the internet message boards to find people with similar problems who have undergone that tx. With a few hours of research under your belt, you’ll have a better idea of whether or not it’s something you want to do.
Sincerely,
Dr. Russ
I believe I have damaged fascia on my lower legs because I feel dents when I rub my fingers down my leg. Then when I stretch a certain way, lumps form on those dents. I used to sprain my ankles all the time playing soccer, and some sprains were worse than others. Defects in the fascia? Muscle hernias. When I relax my leg there are no lumps, only the dents which can be felt.
Tough to say Jon, but could definitely be some sort of fascial hernia (muscles popping through torn fascia as they are contracted).
Sincerely,
Dr. Russ
hello Dr Russ- looking for an idea what is wrong with me – have had pain and stiifness on my left side of body from head neck shoulder hip down to underneath my left foot/heal also more sensitive on left side- have had this for 17 years- symptoms before were neck pain and lower back i have been told that my muscles particularly on shoulder are more developed- i also experienced tremors and panic attacks – doctors diagnosed general anxiety disorder- have had scans to eliminate any injuries- my muscles seem to be in a permanent state of being tight- even my left eyeball seems stiff when i move my eye? any ideas- thanks
simon
Hello David / Simon,
Although Tissue Remodeling might provide a great deal of relief, I would absolutely find a Functional Neurologist trained at the Carrick Institute. If I had a friend, relative, or even a child in your position, this is exactly what I would do.
Sincerely,
Dr. Russ
Dr Russ,
Does all fascia repair its self , if the deep fascia in the back tears under the trapezius muscle , could this repair itself if it splits both sides of the spine .
If fascia tears in the back and an injury to the galea the fascia over the top of the head that didn’t have stitches in at the time could this tear away under the scar .causing it to split
Hello Sue,
You are asking a question that might be better directed at a surgeon. If you literally tear a tissue in half, I may not be the best person for fixing it.
Sincerely,
Dr. Russ
Hi, I had a partial hysterectomy three years ago and the doctor used a laparoscopic robotic devise through four different incisions encircling my belly button.
In order to use the robot, they had to distend my belly with air. Long story short and about 10 different types of doctors and therapists later, it was recently determined that the bulge in my abdomen, which came after the surgery (probably due to them distending my belly too quickly resulting in a tear), which is contained within the circular set of scars, was no longer due to diastasis recti (becuase I did the proper exercise to heal that), but rather to torn abdominal fascia.
I was told the only cure was to have it surgically repaired. What do you say and what do you know about John Barnes and myo fascias release therapy?
I really need some solid advice. Everyone here in NY keeps telling me surgery is the only solution, but I don’t buy it anymore.
THANKS SO MUCH.
Hello Lisa,
Other than the fact that he is famous, I know nothing about him. Personally though, I would try Barnes before I tried surgery.
Dr. Russ
Dr.Russ, Thanks so much for being a seeker of knowledge, and understanding fascial function and adhesions. I went through one year, of trying to end my lower and upper ab pain, and right pelvis, thigh, groin to ankle pain after lifting and carrying an extremely heavy table.down a ver steep flight of stairs..history prior..but no problems until the table trauma…
I have had 4 open ab surgeries..including complete hysterectomy, and two hernia repairs..story is .after 8 Drs, CT,a HIDA scan..X-rays. Blood work, 2 pelvic ultrasounds,, colonoscopy endoscopy…and then I self refered and went to a UroGyno..who did an interior exam.and voila. ..Pelvic floor dysfunction related to Myofascial .this disorder ..is treated by a pelvic floor pt…Readers Digest did a feature called the Pain Down There 10/2014. The pelvic floor is a melon sized web of muscles, ligaments, and exquisitely sensitive nerves at the bottom of the pelvis. It affects a wide range of organs and tissues, the treatment includes massage like work inside the vagina by a therapist to release tight spots affecting the piraformis, and obturator…Pelvic Floor Spasm:The Missing Link in chronic pelvic pain Oct1, 2012 by Patrice M Weiss MD…this is also an issue in men….Herman and Wallace Institute is a great resource..and Urogynecologist Colleen Fitzgerald MD Chronic Pelvic pain at Loyola… It may be hard to find a Pelvic Floor PT….but do research…
It is life-changing and worth it.
Ann
Thanks for sharing Ann,
I have been planning on doing a post on Pelvic Floor Pain. However, because it’s not something I treat here, I have put it off. Thank you for putting this back on my radar.
Sincerely,
Dr. Russ
I was in the gym doing squats one evening where I live human n the south of France. To do improve my performance I wore knee wraps but on this occasion I wore a pair of denim shorts that help restrict flexion at the hip joint thus allowing either more weight or more reps.
The next day I had cross bruising line over the tops of my thighs and groin area where the denim had pressed very forcefully into me. After a few day I had pins and needles in my left groin and after a few more day pain would develop after walking or standing for an hour or less.
My theory is that I have torn the fascia tissue in my left groin. I have no pain when attempting a sit up or bringing my thighs towards by body or addicted pain. I can feel no lump or tenderness in my lower abs to pelvis tendon area.
It has been five weeks now and I take ketoprofen twice daily.
I went to the local hospital in Béziers where I live and saw a specialist. He believe I may have strained or lightly torn the lower an tendon area. I think I have torn the fascia because when there is pain its between the skin and the muscle, not in the muscle.
What do you think?
Hello Nigel,
As an ex-Powerlifter, I sympathize with you, but as far as telling you which specific tissue you tore, I am not sure.
Sincerely,
Dr. Russ
I am 24 weeks pregnant. 6 weeks ago i experienced a sharp pain/pulling on the side of my lower right thigh, just above the knee area. The pain dissolved with walking, but little by little it increased. I went to the chiropractor , as I thought it was sciatica, but the pain came back and worsened. Now it is spread though my side and front thigh, very deep. The skin is super sensitive, walking is accompanied by constant pain/pulling/ tingling. At nights there is burning added to all that. I only get around 3 hours of sleep… My doctor … Is of no use , he told me ta take Tylenol …which does not help enough so I can at least sleep. I am desperate…I still have 16 weeks to go with my pregnancy, but things are getting worse every day. Please help!!!
Hard to say what’s causing it, but definitely nerve involvement (tingling). Could be a baby-pressing-on-a-nerve thing. Just too hard to say.
Dr. Russ
If you were my client, I would try a soft roller. Its excellent. I would start with your back and sides, and then the legs. Most likely the baby needs to move position for you to get lasting relief, but this should help more than anything else to reduce the pain. This type of massage will serve to rehydrate your tissues and allow fluids to move more freely. Nerves get irritated when tissues can’t move. It’s gentle enough to use all over your body barring any positions that are uncomfortable or contraindicated while your pregnant. I wish you the best!
Thanks for the reply Lisa,
I thought about including a link to THIS ARTICLE about “Foam Rolling” I recently published, but was too busy at the time. By the way, Lisa runs 3D Fitness in the Houston, TX area. It’s a personal training and fitness studio that specializes in Pilates and various sorts of Functional Training. Hope that is helpful Rodica. Thanks Lisa.
Sincerely,
Dr. Russ
I am a LMT in AL and have been dealing with forarm and hand /wrist pain presumably from work related overuse for a while (I was diagnosed with carpal tunnel 3 years ago) but it has in the recent past few months gotten close to debilitating. I try to avoid conventional Western medicine as much as possible and use herbs & nutrition as my main/first choice of action but I need to find something else to allow me to continue my daily activities. I am only 30, raising a almost 2 year-old and cannot continue along this degenerative path of hardly using my hands for daily activities at home. I have successfully been battling TN (trigeminal neuralgia) for the past 8 years with magnetic therapy and nerve relaxing herbs etc. I’m so grateful to find your site! I’m unsure if I’m both acute & chronic or where to go for further help healing what I believe is forearm/wrist tendenosis.
I would guess that you are “Chronic” although not necessarily in the hyper-sensitive class. I would also guess that you could benefit from really getting in there and having things really torn up (HERE). Make sure to check out THIS TESTIMONIAL while you are at it.
Sincerely,
Dr. Russ
Con’t …
can’t get my orthopedic surgery to admit that there’s a problem. As your blog says he says nothing is wrong yet says go to PT and the pain doctor. My PT thinks surgically repairing the fascia would help the rope and pulley muscle system work. any suggestions? thank you
Hello Margo,
Tough for me to comment on the surgical repair as it’s not my field. It is not something that is commonly done. There is, however, a second issue in play here. You have got to go to my Doctor Schierling dot com site and start reading my numerous posts on Inflammation and Scar Tissue.
Sincerely,
Dr. Russ
Hi
I am suffering from pain in abdomen area since last seven years. All tests ,scans etc done but no diogonisis. It all started when I tied my stomach area too hard for few days .I kep telling docs that there is something wrong with my abdominal wall and not internal organs. But since no scan shows anything ,I am left suffering with this pain. While researching I found that I have developed a diastis of rectus muscle. But the severe problem is in upper abdomen. I cannot stand beyond 10 minutes and it starts hurting in upper area. I think I have damaged some connective tissue ans fascial with my tight tieing of abdomen. What can be a solution for me. I am too frustrated
I wrote THIS POST in response to an athlete I treated who had nearly crippled himself with pain. I see lots of these types of problems.
Dr. Russ
I am 34, (barely maintaining 97pounds) importantant !! As i have only 5’3″ and weighed close to 140 and very active only 2yrs ago. My diagnosis is interstitial cystitis and chronic pain but i also have muscle loss on the right side of about 75percent( 55on left) frequent mri and ct scans do not explain pain not related to ic , until i happened to run across. An er doc who practices orthohealing !!! And told me my fascia was so tightly woven it was the cause of the pain !!! Eurika. I found a logical answer finally 🙂 !!!!! I don’t. Believe in masking pain with drugs unless there is a surgery (broken bone protruding lol, organ removed hahaha. , etc) so he showed me some resetting techniques for home that are helping tremendously! Glad i found a site to reinforce what i was told yesterday at the emergency room , thank you for the information
Hello Julie,
There could be more to it than that. Make sure to read THIS POST on the topic as well.
Dr. Russ
I’ve developed L’Hermitte’s sign and just underwent a whole MS work-up. I started with plantar fasciitis years ago…then had a frozen shoulder, now all sorts of pain related to what I describe as tightening of all my joints….especially my back and neck. Thoughts????
Hello Elizabeth,
I have written quite a bit on my site about MS. HERE is one of the posts.
Dr. Russ
Very good blog today, thank you. So these tender points on my spine could be caused by fascial adhesions?
Thank you Derek,
I would be shocked if they were anything other than some sort of myofascial problem — either Fascial Adhesions or Trigger Points (my money is on the former as you get below the upper traps).
Sincerely,
Dr. Russ
Just wondering how u would treat a fascial tear. I have a 5.1cm tear of the fascial around my gastroc. Thanks
Hello Chris,
I’m not really sure. The Fascial Adhesions I speak at length about are the microscopic “tears” that produce Scar Tissue that can’t be seen with diagnostic imaging such as MRI. You are talking about a two inch tear in some of the denser Fascia in the body. Not something I could likely help.
Sincerely,
Dr. Russ
I’ve been dealing with shoulder, neck, scapular/thoracic pain for almost 10 yrs which has progressively gotten worse, it’s debilitating. I’ve exhausted all my options, X-rays, MRIs etc… No Dr can ever figure out what’s wrong. I believe in my heart that it’s fascia related. I’m only 34 yrs old and I’m in severe discomfort. I wish somebody could help me, living life is a daily struggle.
Hello Derek,
TODAY’S BLOG POST might be worth reading.
Sincerely,
Dr. Russ
Have u found any answers. I have researched my left side pain for ten years and came across this thread. my issue has always been on my left side; specifically thoracic, neck, shoulder, hip, and front left area of my shin. Have found no answers. Doctors can’t find anything and tell me I am stressed. So frustrating. Im so tired of this.
Your’re right Susan, it’s extremely frustrating. Make sure to take a look at my video testimonial page at DoctorSchierling.com.
Sincerely,
Dr. Russ
Have you ever heard of kenalog being injected into an abdominal muscle and damaging the fascia causing a huge herniated muscle?
Hello Donna,
I have personally never seen this happen at the ABDOMINAL MUSCLE, but CORTICOSTEROID INJECTIONS are notorious for destroying / degenerating Collagen-Based Connective Tissues.
Sincerely,
Dr. Russ
Hello Dr. I think with your help I may have identified the problem I have. For the past twelve years I have suffered very bad stabbing pains in my lower back, neck, shoulders, collar bones and sternum. The locations keep changing weekly or monthly. The specialists have yet to figure out what’s wrong with me. They keep giving me steroid injections. M sternum hurts so bad right now I have to hold my breath while I write this. I live in east stroudsburg PA. I tried exercise, physical therapy, aqua therapy. Is there anything I can do to reduce the pain? Or even dare I say it, Cure myself? I am on ssd, 35 years old and stuck in constant pain. I can’t do anything. Thank you for all this information anyways. You sound like a doctor who really cares.
Hello Johnathan,
You can try THIS, but my best guess is that you’ll have to deal with the adhesions.
Dr. Russ
Hi- I’ve just been diagnosed with a facia tear on my hamstring (a 7cm long x 5cm wide lump that appears on my right leg under tension- then virtually vanishes when I relax) it doesn’t actually cause pain where this occurs but the rest of my hamstring really aches or often throbs. I had knee surgery last October (2013)
Hi- I’ve just been diagnosed with a facia tear on my hamstring (a 7cm long x 5cm wide lump that appears on my right leg under tension- then virtually vanishes when I relax) it doesn’t actually cause pain where this occurs but the rest of my hamstring really aches or often throbs. I had knee surgery last October (2013)
Hello Mr. Arrowsmith,
This sounds more like a herniation of the Fascia as opposed to the microscopic tearing that I am talking about on my sites.
Sincerely,
Dr. Russ
Is there any way of fixing a torn fascia without having surgery?
It totally depends on what your definition of “torn” is. In most cases, I would say yes.
Sincerely,
Dr. Russ
Since you have seen these at the injection site are they typically removed?
I’ve never seen them removed.
Dr. Russ
Just found your site and piriformis syndrome may be what I’ve been dealing with for 30+ years. About 5 years ago I had some marble-sized lumps appear in the ‘triangle of pain’ area. An MD said they were ganglion cysts (I have one on my right wrist) and a chiropractor said they were fatty tumors. They are harder than the ganglion cyst on my wrist, but not extremely hard. All my life I’ve had small gravel-like bumps in the tissue around the outer sides of my ankles. Sometimes there is aching and mild pain in these “lumpy” areas. If I massage them there is a mild burning sensation. The lumps are not visible, they can only be felt and they do move around some when massaged. Could these lumps be fascial adhesions?
Hello Patty,
Highly doubtful they were Bible Cysts on your buttocks (they are common on the wrist). And usually Lipomas (fatty tumors) are fairly soft. Not sure what it is, and it may not be related to the pain you are having. They do not sound like Fascial Adhesions or Trigger Points, although the latter would be more likely than the former.
Dr. Russ
I have had chronic pain in my left heel following plantar fasciitis well over a year ago. I had a few cortisone injections during my healing period. The plantar fasciitis pain was gone but I soon realized I now have a marble size hard knot inside my heel were the fascia connects.
First the doctor said it was liquid filled and injected it more saying it was just inflammation then he followed with oral steroids for 14 days. I finally went to a new podiatrist an he looked at it with ultrasound and said it is solid and he would do a surgical injection that may help it shrink. Still no luck and a lot of money spent. Now my doctor wants to cut it out and that really worries me because if it’s scar tissue won’t it just possibly come back after a surgical procedure??? I’m at my breaking point and just don’t know what else to do.
I can’t even find anything to read online about this particular situation and really do not want surgery.
I certainly can’t tell you what it is, but I have seen these before at the site of CORTICOSTEROID INJECTIONS.
Dr. Russ
I am a guitar player and developed pain in my palms after extended practice sessions. I feel small, painful lumps in the muscle of the palm. This has persisted for six months despite rest,ice, and NSAIDS. What are my treatment options?
Hello Shawn,
THIS is probably what you are looking for.
Sincerely,
Dr. Russ
Hello Doctor. I just want to thank you for the article on understanding fascia. I was in Boot camp in 2013 and couldn’t make it through because of how much pain running/speed walking brought me. The physical therapist there actually was the first doctor I had went too who had figured out what it was that was causing me the pain. The tears in the fascia of my shins. Its gotten worse over the year as well. Do you have any suggestions? Its getting to the point that regular walking on hard surfaces is making my left shin throb where a majority of the pain occurs.
Hello Tyrone,
You are describing SHIN SPLINTS.
Dr. Russ
It comes and goes. I was told it was fascia tears. It feels like my legs are never going to heal.
Hello doctor,
A few years ago I pulled a muscle in my right lower back pretty bad. I heard that “pop” sound. After 2 months of increasing pain I finally saw a doctor who gave me muscle relaxers and nsaids. The pain definitely died down but over the years I was in a cycle of healing and re-injuring that muscle. About 2 years ago, I did something to it and I can now feel the ruptured muscle in my back as there is a ball/lump where the muscle rolled up and I can feel a frayed muscle underneath when I compare it to my left side of my back. There is noticeably less muscle tissue in that area as compared to the left side of my back and all those muscles feel like hard ropes compared to the left side of my back which is soft and smooth. Ive ben doing physical therapy for a while now but this injury is still in a slow decline. Im afraid I could be very disables by the time im 40. Im 32 now.
Hello Nick,
Go to my Doctor Schierling site and check out my stuff on THORACOLUMBAR FASCIA.
Sincerely,
Dr. Russ
Very informative. I’ve been having problems managing the pain from costochondritis off and on now for 18 months. The chiropractor I see explained the fascia connection with the cause of the pain. The massages and ice/heat packs do help, but for just a few days. I was diagnosed with fibromyalgia about 10 years ago. I did fall on my chest 2-1/2 years ago. But, just a bit of pain from the fall that required ibuprofen for a couple of days.
Are there any exercises to help heal the fascial adhesions?
Thank you,
Karen C.
Hello Karen,
I do a lot of specific work with RIB TISSUE PAIN, CHEST PAIN, and ABDOMINAL PAIN. Unfortunately, Costochondritis is an Inflammatory problem. Make sure to read my numerous posts on INFLAMMATION for information that will help you solve this thing.
Sincerely,
Dr. Russ
Hi dr Russell,
First of all thank you so much for this great information. My question is related to this. I’ve been struggling with abdominal issue for 5 years. From the navel to ribcage I feel constant burning or inflammation. I have some days when I feel less or more but this sensation is with me 24/7 365days for 5years after I had heavy antibiotics due to nose surgery. Doctor’s didn’t find anything in tests and tell me it’s in my head. i feel more inflammation when I move or bend my stomach to side ways.i feel minor bumps when I squeeze my stomach and touch with finger. Sir, do you think this could be abdominal adhesions?
Hello Jas,
First, I would go over to my DoctorSchierling dot com site and start reading. Lots of info on this topic. Inflammation always leads to Scar Tissue, and antibiotics wreak havoc on your Gut, where 80% of your immune system lives. In other words, antibiotics can cause great amounts of inflammation. Make sure to look up my articles on Abdominal Adhesions while you are at it.
Sincerely,
Dr. Russ
Dr. Schierling,
I am a 39 yr old female who has been “shrinking”. I feel as though my whole fasciae is pulling me into the fetal position. I no longer eat wheat, dairy, refined sugar or food additives. After battling chronic yeast, 2 c-sections and losing mobility in all joints, the deep tissie massage was the only thing that has offered relief although I am unable to miss more than a day of massage or I
go back to “shrinking”. What is the prognosis for fascial healing? Do you believe there is a conection between yeast and fascial deterioation and adhesions?
Holly
Hello Holly,
Not sure that there is a direct connection per se between YEAST and Fascial Adhesions. However, there is a direct link between Inflammation and Fibrosis (Scar Tissue). Once you grasp how inflammatory yeast is, the leap is rather easy (HERE). This sounds almost like PAM ARNOLD’S case.
Sincerely,
Dr. Russ
Dear Dr. Schierling,
I have been suffering from what I was told was bursitis in my hips, bilaterally, for over two years. I was doing mini-triathlons and possibly not training or stretching properly. I am in physical therapy now and have been off and on for a year. I cant seem to get rid of this pain. My physical therapist tells me my IT bands are a mess and they are terribly sore to the touch and very ‘lumpy’. If I keep foam rolling them and have them do manual work to the IT band to break up the scarring and adhesions do you think this will help thee hip pain?
Vicki
Hello Vicki,
Not that Foam Rollers are a bad thing, but if they were truly effective for these types of problems, you would not be posting to my site.
Sincerely,
Dr. Russ
Dr. Schierling,
Thank you for the site, Its the best starting point for me regarding rethinking therapy for the Plantar fasciitis adhesions I have in my right heel. I go through chronic pain everyday, and I need help. In June I re traumatized the area with blunt force from a small sharp rock. Two years previously I also struck a rock on the same spot it seems. From the first injury I suspect the adhesions didn’t fix themselves (don’t know how else to say it ..sounds dumb right!) but I’ve been able to mask that pain with quality footwear and swap 2 pairs of Paris brand orthotics which as you’ve said Orthotics replace the arch. In hindsight I guess it improved but after this June bout however the two separate Sports Medical Dr.’s I’ve seen in my area of Winnipeg Manitoba, recommendations differed. The first Dr. said swap out the orthotics for “soft ” support so I’ve been wearing Tuli Heal cups in all my different shoes and doing all the stretching, including plie’s actually because the calf dips over the edge of stairs just seem to aggravate the tissue. Scrunches work, writing out the alphabet with my big toes over the edge of the bed before I get up are OK but not a day goes by wherein if I’m on my feet for more than two hours I’m in Chronic Pain again and again. I received 6 LLL therapy sessions (passive low light laser therapy, not normally covered or recognized by health plans and it was more psychological than anything else). The second Dr.’s opinion was to stretch out the fascia and thumb message the arch the instep, but stay away from the heel and keep the foot taped everyday in such a manner to gather the fat pad as well but it just doesn’t work well enough to relieve that pain that comes back. I thought maybe I had Bursitis because I’ll be driving and out of nowhere BOOM the pain will emanate from the fascia through the ankle and deaden in the shin area. I have a short term medical form which protects me at work , otherwise I could be required to be on my feet all day. Do you know anyone that can perform this procedure of remodelling my tissue here? I’ve checked your picture page and I can’t fathom how this could be done to a heel without having me tied down? I’m willing to try it because it makes sense now that I’m just re aggravating. In the meantime I’ll try the stretches for this area as described on your stretch page and research the anti inflammatory collagen enriching foods page.
Hello Dwayne,
Yes, a rock could easily cause an adhesion. I am not a fan of “soft” orthotics for most people because they do not provide enough support. The heel never bruises like shoulders or other body parts do. Not sure who to send you to in your area.
Sincerely,
Dr. Russ
2 years ago my son was in a very bad car accident. At the time he was in excellent physical health. He hit the steering wheel with his face (he did have a seat belt on) broke his nose and suffer some brain trauma. His back hurt but that was ignored. Well it has progressively gotten worse. He is in the military and not able to work due to pain and swelling. He has been doing physical therapy including water therapy, trigger massage weekly and now chiropractic has been added. His shoulder, especially lower back, (most of his back actually) is very painful. He has experienced numbness tingling in his arms, hands, legs, and feet off and on. If he misses a week of the very painful trigger massage it is far worse. Everyone treating him has said the muscles in his back are constantly extremely tight and won’t let go and relax. His core strength was fabulous now horrible. The massage therapist feels he is dealing with adhesions. Because he is considered injured the military will not allow him leave. He has had MRI’s, xrays, and back/head scans all come up clear. He is in El Paso, TX. Is there anything you can suggest? Much of what has been done that works we have had to pay for out of pocket. He just wants the pain to go away. Thank you!
Hello Valerie,
MVA’s are devastating, and in my estimation, account for more CHRONIC WHIPLASH PAIN than everything else combined. Unfortunately, the military has always lagged behind when it comes to taking care of chronic problems like this. HERE is an example. I wish I could convey to you how bad the person in this link was. He wanted to do a video, but is unfortunately tangled up in litigation pertaining to his injuries.
Sincerely,
Dr. Russ
I am so well aware of the military lagging behind in care. The military chiropractor they sent him to put his hip back and then did 2 or 3 treatments of electrode therapy which was just a duplication of the physical therapy appts he was also having. No other adjustments were even made. It is why I am paying out of pocket for both a real chiropractor and a weekly trigger massage. I would love to bring him to you but the military will not give him a leave due to his injury. He isn’t even allowed to come home. I must therefore seek outside of the military care for him in the El Paso area. Any ideas in El Paso or self treatment things he can do?
Hello Valerie,
Other than making a concerted effort to deal with SYSTEMIC INFLAMMATION, I am not sure as I know no one in your area.
Dr. Russ
I was a sprinter in high school & was running in college before a massive achillis tendon injury occurred. Since that time I have experienced tightness in my hamstrings. How can I break up the fascia correctly & regain elasticity again?
Hello Po Daddy,
Try a foam roller. Often time it is difficult to break messed up tissue on your own.
Dr. Russ
I have been in a lot of pain and discomfort for a long time. My back and shoulders are full of knots and lumps. I went for a massage and was told that my fascia is really tight all over. I have been diagnosed with scleroderma which effects the collagen in the body. I have no skin thickening but I have muscle pain and a feeling of weekness. Would scleroderma effect the whole fascia and be a cause of this tightness and pain? Any advise would be most welcome.
Absolutely Scleroderma could cause pain and tightness / restriction! Scar Tissue Remodeling is not the solution. Because this is an AUTOIMMUNE DISEASE, you need to do things to help ‘fix’ your Immune System. Click on the link and spend a few hours reading. You may be overwhelmed at first, but the information is invaluable for people with problems like yours.
Sincerely,
Dr. Russ
I recently went to a chiropractor that left me in more pain! Before even looking or feeling the area I was concerned about he told me I needed to have the Fascial Adhesion to be broken in my back and shoulder where I was having shooting pain. He used hard plastic scarpers across the muscle areas and said it would make a big difference in that area within a couple hour. the next day I was in tears from the pain and for several days later. Now a week later I have muscle weakness and struggle to reach up my arm above my head. Do you think he damaged the Muscle Fascial and if so will it heal over time???
Hello ENF,
It always amazes me when a physician of any sort prescribes or treats without really understanding what is going on first. I realize that many cases can be extremely complex, but how can you help someone without at least having some sort of idea of what the underlying problem is? As to your particular case, it is tough to know exactly what happened here or what is going on right now.
Dr. Russ
I have done yoga for years. a few years ago, I overstretched where the hamstrings attach to the sit bones. I start stiff every morning barely touching my toes. At the end, I can put my hand flat on the floor with my chest on my leg. Then the next morning the same thing and then after a half hour of hamstring stretching I can do it again. It hurts at the attachment. Why so stiff? I also have a Baker’s cyst behind my right knee sp the more exercise, the more it swells. I never gain on the stretching. Why?
Thanks
Hello GBSK,
Sounds like HAMSTRING TENDINOSIS. HERE is an explanation of why stretching is not always the be-all end-all it has been made out to be.
Sincerely,
Dr. Russ
I think I have finally found the root of my pain problem after over 20 back doctors. My massage therapist thought I had a rib out of alignment so sent me to chiro and sure enough. But pain is still on my right side, so she is thinking the rib fascia has adhesions or scar tissue because I have had the pain for over 7 years, so she and the chiro will work together to see if they can correct this situation. That would be WONDERFUL> I’m so ready to be off ibuprofen and tramadol. Thank you —so glad I found your info.
Pam
This is a very informative piece. My question for you is this: would working out in water be advantageous to maintaining better mobility and strength in the muscle tissue if chronic pain likely associated from the Fascia is the likely cause? Is this an option to manage the symptoms of chronic pain versus just taking a drug? Thanks much and really appreciate the simple to read explanation.
Hello Lee,
Working out in water can be fantastic. However, it is no substitute for having the Fascial Adhesion deal with.
Dr. Russ
I have recently learned I have severly torn my plantar facitits and on a MRI scan the Dr. Told me it just looks like a bunch of strings hanging there. I did not have a tramtic fall or do anything to my foot. Was having pain for months then he put me in a boot which made me much worse then now to a cast once he read my results. This Dr seems very uncertin in what or how to treat me. He has only said it should heal eventually and I should have no more pain in my foot from the plantar facititus. On the other hand when he took cast off once it feels like I have a towel rooled up to one side inside my foot as well as under my pinkie toe the bones are so sore it almost feels like they are going to break through my skin. Another Dr said she had heard of fixing this with a band to stabilize my foot. Any suggestions I am really at a loss here since this Dr seems very uneducated as how to deal with my injury. All I have read states I am in danger of other problems down the line coming into play once the arch is gone for good.
I would make the trip to see Shawn Eno in Idaho Springs, Colorado (Xtreme Footwerks).
Sincerely,
Dr. Russ
Dr Russ,
Please can you tell me is fascia tough?
if it is torn in half can it repair its self or would you need surgery, the fascia down the middle of your back in the thoracic area the fascia that goes down covering your spine?
Yes Sue,
Fascia is extremely tough. It does repair itself. However, trying to determine whether or not your particular problem will fix itself is impossible for me to say.
Sincerely,
Dr. Russ
I am mainly right handed but use my left when my right is out of commission. I also have double jointed thumbs. Lately, my right shoulder down to my elbow down to my fingers has been very painful to move. I went to the doctor and he told me that I have just worn out my arm. I have been a gardener all my life. I am 50 yrs of age and garden on the weekends. I refuse to believe that. Where do I start to find out what is really wrong?
Hopefully you live nearby?
Dr. Russ
After a extremely jerking traumatic fall off our cruising sailboat,in which I over stretched my arms, abdomen Rt. Leg and especially lower back and sacroiliac area I am having myofascial pain syndrome problems as you describe to the “T”. Also have muscle knots in which I have been treated
by trigger point injections for past 7 yrs. Probably at least 500 injections overall. One year after fall I had a ruptured disc L-4-L5 fixed with a discectomy and have a couple more bulging discs in the lumbar area.
Presently am experiencing the tightness and taught bands as you describe. Am constantly using balls,foam rollers,hard surfaces etc., to get some relief.
Am retired X-Ray tech. And Ultrasonographer. Much research and diagnosing of muscles being done in Ultrasound right now but have not seen articles in journals on myofascial issues. Only MRI elastography seems to have some promise,but this is still in the research phase. Used primarily for organ fibrosis especially in cirrhosis of the liver and tumor
Rigidly. Hopefully will also be able to tell fascial stiffness or tightening too.
Mayo Clinic doing a lot of the work .
My questions to you are: Am I doing more damage to fascia with pressure Thx.? Does this seem to be a familial problem? Finally does stress and
Elevated cortisol and the consequential biochemical cascade effect this
Syndrome? I’ve been told to do Yoga and maybe biofeedback may help.
Also does multiple needling in the stiff tissue-possibly bring some blood perfusion to thickened fascia.
Chris.
From Michigan,USA
Hello Chios,
Pressure on the Fascia as a form of treatment has been around just about as long as the human race. The needling technique you are describing here (“Dry Needling”) helps many people. And finally, ADRENAL FATIGUE does not do any favors to anyone or any healing process. Make sure you check out TODAY’S POST, as it has application to your question.
2 weeks ago I started getting sharp shooting pains in my arm, the front bicep area, when I move my arm out to the side. I rested, iced for about a week with no improvement. Went to the doctors, they said it was most likely tendonitis in my shoulder and gave me a shot of cortisone. That made the pain worse. Now its five days after the shot and the pain is still the same sharp shooting in my arm. Someone mentioned it may have to do with the fascia. How would you know if it was fascia vs tendonitis?
Honestly Sarah,
Sometimes I do not know. Also, it is common that people have both. The cool thing is, since these two tissues are extremely similar to each other, I treat them both in similar fashion. It is not really important to be able to exactly differentiate the two.
Sincerely,
Dr. Russ
I had L5-S1 fusion, disctectomy. My surgeon said that I didn’t have the fascia that connects the muscle to the bone, so they had to tear it off to operate. Help me please. 6 months post op, and having problems with no answers. December 3/2014 was surgery date, Dr. A. Woo was my ortho surgeon.. From Saskatoon, Saskatchewan.
Hello Judy,
Sorry, but not sure how to answer this. They tore it off — it’s gone. Not sure what all that entails or means to you.
Dr. Russ
I had spinal surgery 21 yrs ago for scoliosis repair with fusion(T12 – L2/3) & I have now suffered with chronic low back pain for 20yrs. Loads of pain at L2/3, down side & back of right leg with huge pain directly next to shin bone of same leg. My right SI joint will not stay where it should and causes me massive grief. All I can say I wish I could see you Dr. Schierling. Dr’s in Australia give me the blank stare & I’ve tried everything & I’m also on disability & on meds 24/7 just to keep me upright. This site tells alot.
Hello Andrea,
Thank you for your comment. Trust me when I tell you that the “blank stare” issue is not confined to Australia, America, or any other country. It is extremely widespread.
Sincerely,
Dr. Russ
25 years with a problem that remains undiagnosed after many doctor visits. I have been told to learn to live with it and take more depression medication by doctors who do not understand my symptoms. I have constant pulling, spasming, groin pain on the left side. It also pulls internally on that side and if I let, it the left side of my mouth joins in and strongly pulls in rhythmically. I also have nerve electrical type sensations in the sole of my left foot. I have scarring from an episeotomy on the left after childbirth 40 years ago. The muscle at the top of my left leg is tight. I also sometimes feel a sharp stinging pain on the left internally in the gynaecological area and sometimes in the bowel.
The doctors say that there is no known link between the areas that I have mentioned.
Does this all sound like fascial scarring? I am in the UK.
Kind Regards
Emm
Hello Emm,
All I can say is ‘wow’. I have never heard anything quite like this before. The pulling from the mouth is particularly interesting. As you what this could be, I would be amiss to tell you that I have any real idea. Fascia acts as a second nervous system (HERE). One of the problems with some Fascial Adhesions is that there is almost no way to get to them. I wish I could offer you something better. I would consider seeking out a Functional Neurologist trained by Dr. Ted Carrick.
Sincerely,
Dr. Russ
Could you give me your opinion. My son was a very fast sprinter, football player, and could build muscle mass very quickly. He has very large bones and was easily the strongest kid in school entering high school (absolutely no steroid use!). He started experiencing extremely tight hamstrings when he ran and had to give up track. He went to several doctors that prescribed just stretching and physical therapy for muscle imbalance. It only got worse. Finally went to an orthopedic doctor and MRI showed extreme bone marrow edema in pelvis. He was on bed rest for 4 months it was so bad. He recovered but pain and tightness happened again as soon as he started athletic activities. Rest again, happened again. Rest again, happened again. We don’t know why this keeps happening. He watched a short video about myofascial release using a cue ball shoved and rolled into his hamstrings. He tried this therapy after he started experiencing a lot of pain again. Almost instant relief which makes me believe it is a problem with his fascia. Are there other treatments to keep this at bay or are there diseases that can cause this.
Hello Lyn,
There are dozens — maybe hundreds — of different ways of dealing with Myofascial problems. Bear in mind that sometimes these fascial issues can be systemic (HERE).
Sincerely,
Dr. Russ
Hi there, I am a 37 year old male with a burning pain in my left lower side after an appendix removal. I was diagnosed with inner coastal nerve damage and have gone threw 3 shots of nerve block in my back. Back surgery to cut the nerve bundle. And things have only gotten worse! Dose this sound like fascia issue? Please help! Thank you!
Hello Robert,
Impossible to tell, without looking at you but it certainly could be.
Sincerely,
Russ
I am sorry I forgot to ask can muscles, tendons , subcutaneous tissue damage be seen with ultrasound or mri when I said subcutaneous tissue I meant the skin layers including the fascia
thank you
Sincerely,
Yes to muscles and tendons, “MAYBE” to Fascia and other tissue.
Dr. Russ
please can you tell me my Dr is wanting me to have a scan to look at the fascia and muscles and subcutaneous tissues of my back to look for serious damage , he said he thinks ultrasound ,its the thoracic area it feels like the tissues in side are splitting , can you also tell me where fibrous connective tissue is found what is it, is it fascia ?
Hello Dr. Russ,
My husband had a surgery “green light” 3 years ago. He is still in severe pain, as a result of the surgery. Could you give us consultation to help?
Sincerely,
Zoya.
I assume that this was for BPH? Doubtful I can help but send me a history to my Contact Page and I will take a look at it.
Dr. Russ
Hi Dr.Russ I believe I need the treatment you described badly. I had my gallbladder removed after my first pregnancy which left some sensitivity on the right side and back but I was fully functional. I then had a second pregnancy that ended in a very complicated c section and ended up eight months later with an appendix removal with witch I ended up with peritonitis, a collapsed right lung, severe hemorrhage and an access in my abdomen that had to be drained. Just to note this doctor also cut my psoas muscle right under my ribs to make sure there were no problems behind it. I ended up with severe pain in my SI Joint and from the front through the back and down my spine at about the T6 level. After just about every test and treatment and a surprise third pregnancy and c section they finally concluded that my SI joint was torn and they put a very long screw through my hip and spine to stabilize it. I am now in my fifth month of physical therapy and can walk very well now but I have been told that my lower ribs are actually immobile and the fascia wrapping around my right side is so
tight it can’t even be pushed in. It is the
muscle fascia now that is causing me so
much pain and the therapist has been trying
multiple manual methods to break it up but we
have made little progress. I was just thinking
about trying acupuncture because I don’t
know what else to do. I am at the point now I
would do anything to get this fixed and feel
better. I have been almost immobile for three
years am 37 years old and have three small children that need me desperately. In reading your article I finally felt like finally someone understands and has a realistic idea of how we might really fix it. If there is anyway I can be part of this therapy it would be worth it. Even if I had to travel. Can you give me more contact information on where to go and how I might go about getting this treatment?
Thank you for anything you can do.
Sincerely,
Rachael Simpson
Hello Rachael,
I see lots of problems around the PELVIC GIRDLE, RIBS / CHEST, Abdominal Wall, and others. Cutting the Psoas could be a problem depending on what was done. My contact info is HERE.
Sincerely,
Dr. Russ
Hey doc, I know this may be unorthodox, but I found you on the Internet, and believe you may be able to give some insight on my issue. I’m an athlete who suffered some type of bicep injury, but no one locally seems to be able to diagnose. There is in fact a deviation in my bicep, but there is zero pain, and no brushing or swelling. I have a pic that I sent to your personal Facebook, not the business Facebook, as I could not send a pic to that profile. I can email it as well. Could you please share your thoughts on this? Thank you sir.
Email it.
Dr. Russ
I am in physical therapy for fascia
Restriction, I have several lumps, my OD.
Has been treating me by using his thumb to push the lumps back through the fascia. My left hip and actually my whole left leg is affected. My left knee is extremely painful. I had an exray of my hip which showed only mild osteo arthritis. Even with pt I am in extreme pain, can barely walk orove my left leg. My bands of muscle through my left leg restrict
My movement severely and cause extreme pain. Would your treatment be more productive
For me?
Probably.
Dr. Russ
Hi Doc Schierling!
Thanks for your website! I have already heard a lot about the importance of fascial tissue but your article really puts it straight!
I have a question:
Do you think a tendinosis can be the reason for the swelling of a whole joint. In my case, it is the knee.
I am a professional tennisplayer, suffering from pain in the back of my knee starting a year ago. It started with stiffness in the morning, but after a good warm up I was able to play without any pain but at some point i was feeling it on court, so i had to stop and rest.
The pain showed up irregularly for the next time. MRI no diagnosis.
I remember doing leg curls on a gym ball and ultimately my knee got swollen.
Another MRI showed that there was nothing wrong regarding the knee.
I was more or less treated for an IT Band Syndrome, whereas I do now think it has much more to do with the Hamstring tendons. Still i got a lot of bruises on my IT-Band..
The swelling got away, it took a while though. I worked a lot on my core stability and my strenght got much better. It took me more a less 6 months to start to play again.
The only time i still felt pain in the back of my knee was when i was accelerating, e.g. sprinting from the baseline to get a drop shot (i felt it not right from the beginning but after 2-3m, so I have to stop). I sometimes feel stiff the next day when i was training a lot. But foam rolling is a big help. Apart from that and the sprinting i felt okay!
More suspect for me is now that after competing in a tournament, my knee got swollen again !
Thats why I wanted to ask you: I was reading your other arcticle as well..
What do you think of all this, are these signs for a tendinosis? And what about the swelling? Is there a connection or are there other things that should be considered?
The last time it was swollen, the MRI did not show anything regarding the knee and also the doctors were running bloodtests, analysed the liquid in the knee, etc. so it should not be systemic.
Thanks a lot!
Julia
Germany
Hello Julia,
Although you may have Tendinosis, this problem in and of itself is not going to cause swelling of the entire knee. Many people have multiple problems. If a foam roller helps, your problem is likely Tendinosis or FASCIAL ADHESIONS. Add some COLD LASER to whatever protocol you are doing.
Dr. Russ
I have fibrous connective tissue , collagen ,and adipose cells coming out of an oral fluid all of the time , I have had acupuncture to my scalp and my scalp has a fluid movement over time the fluid has come into the oral cavity
I don’t know what has happened the fluid is gel -like its awful can you help me this isn’t right is it who can I turn to
Hello Sue,
No idea.
Dr. Russ
Terrific article! I have Ehlers-Danlos Syndrome (Classical) and live in Australia. I had to self diagnose to get some answers, as I saw specialist after specialist who just didn’t look at the ‘big picture’ and therefore completely missed the underlying issue! My mother and sister too have EDS. Have you had much experience with any EDS patients and fascia issues?
Hello Bianca,
What you are describing would fall into THIS CATEGORY,
Sincerely,
Dr. Russ
Hello Bianca,
Just wrote an article on the subject.
http://www.doctorschierling.com/blog/ehlers-danlos-syndrome-tissue-remodeling
I believe that I have Duputren’s Disease. This is seems to fit your conception of adhesions on the fascia. I have the adhesions in more than the normal places discussed in most of the literature and websites. In addition to the adhesions, the fascia or tendons in the region are very stiff. I wake up in the morning with one hand in a fist and the other hand will not fully make a fist. Also having some problems on the back of my hand – stiffness and pain and wondering if it is also some problem with the fascia (do not feel adhesions on the back of the hand). BTW I have none of the pre-existing conditions for Duputren’s.
Hello Anna,
There is always the possibility that you are dealing with a SYSTEMIC PROBLEM. Take appropriate action and find someone who can address our hands.
Sincerely,
Dr. Russ
Wow! I have been suffering for several years with what I have described as muscle knotting. It is painful and will show up almost anywhere on my body anywherefrom pea size to softball size. I have been to many doctors my primary physician has labeled it chronic pain syndrome the rhuemotologist told me I have fibromalgia until I showed up the day after I had a knot on my shin which could still be felt (not as much as day before). She exclaimed “oh…you do not have fibromalgia…I m not sure what you have but its not fibromalgia” She the then sent me for a series of blood tests and never came up with any answers. Prednisone seems to help make it tolorable but my no means is it good. I have also had 2 surgeries where the have removed “fibrous banding” from collar bone area and my elbow I have severe atrophy and nerve damage to my hand. I say this is all related…which none of them will even give a second thought to. Your article is the most relatable thing I have ever read. Where are you located?
Hello Cynthia,
Although I do not believe this is Tendinosis, read this article I wrote on SYSTEMIC TENDINOSIS.
Dr. Russ
Hi I have pain in my glut region which is unexplainable and a have recently started breaking out in unexplained bruised to the right of my knees, and on the outerside of shin near my ankle. Could this be the result of fascia damage?
I found your article extremely interesting.
Nicola Australia
Hello Nicola,
I suppose it could be, but honestly, this is a bit different than what I am used to seeing. Without looking at you, it’s too hard to say.
Sincerely,
Dr. Russ
In March of this year I contracted necrotizing fasciitis internally, in the left side of my neck.
I also got sepsis and bactaremia systemically. I now have pain throughout my body, especially smaller joints, wrists, elbows, knees, ankles, as well as pain in what I thought of, previous to reading here, as muscles…I believe the information in your article is more accurately explaining the situation. Can these types of illnesses, and/or the high levels of antibiotics administered, and/or the atrophy experienced, be an injury that would affect fascia?
Hello Mary,
I have some great info on Antibiotics on my other site (HERE). The answer is yes, both antibiotics and the damage itself can affect the fascia. Whether or not Tissue Remodeling can help remains to be seen.
Dr. Russ
After a fall snow skiing 10 years ago…. Trying every therapy possible… 2 surgeries…I am still in chronic pain… Quit my teaching job 2 years ago due to pain. I have read lots about fascia and know and understand this is my problem. It is mainly in my neck…. Pulling and tugging all the time. What can you do to help me? Otherwise I am healthy and happy…. Just so tired of a pain only a few understand.
Hello Danita,
I can probably help you. Since you are so close (only a four hour drive), you may as well come find out. Make sure you check out my recent Blog Series on CHRONIC NECK PAIN. While you are at it, watch a few of our VIDEO TESTIMONIALS as well.
Sincerely,
Dr. Russ
Awesome information. Are there other doctors privy to this meaningful and life-changing information? You should be conducting seminars around the world!
Thanks Trina,
I am just a guy trying to help as many chronically ill people as possible in my small area of the world.
Thank you for the write-up! I work with chronic tension as well and there really is an astonishing dearth of formal medical study on the processes involved- I’ve had good luck with Canadian journals in particular, but not too much else. Would you mind terribly posting some of the sources for this post? It fits everything I’ve heard and learned through personal experience, but I’d still love to see who did the research and how.
Thanks again!
Hello Corey,
I would give you my sources, but I made them all up. Just kidding. I have a lot of similar material on http://www.DoctorSchierling.com, much of whick is referenced. Hope that helps.
Thanks for the comments
Dr. Russ
I’ve long worked with this issue myself (4 car accidents, arrghghh!!) and am very interested in your approach as i have both found good bodyworkers and developed my own approaches as well. So thank you!! and i will keep reading. But! a quick question: friend just had a slip and fall injury, they thought cracked ribs (and KNOW bruised spleen) but after a week of not seeing rib fractures they went right to very strong physical therapy. His pain level skyrocketed, and my sense is that the original issue is actually fascial tearing. While i understand the micro-adhesions need to be broken and the fascia realigned, this seemed far too soon for me and i believe they are further disrupting needed initial fascial healing. Do you have a timeline as to how long the fascia and systems need to have, to engage their own healing processes, before moving on to the bruising and pain of re-aligning the fascia? I would have said to wait 3 weeks for basic healing (and work gently on range of motion etc) before vigorous massage/PT – what is your experience? Thanks so much!!
Honestly Valerii,
Everyone is so different, it is almost impossible to try and quantify the answer to your question. I look at each person differently and determine their healing capabilities as well as their pain levels, and work from there.
Sincerely,
Dr. Russ
I was Rolfed 25 years ago and these 10 sessions ruined my life! I feel like I am in a straight-jacket connected to a vise and have not had any positive changes at all in this time.
Interesting Gerald,
I have heard that Rolfing is rough. Never experienced it myself or even seen it done.
It really makes sense. Have had rib pain for months on right side. I’m cancelling the tests the doctor ordered and finding a chiropractor who understands the fascia connection.
I am 29 and i just got diagnosed with having a form of Fascia today. Explains a lot actually. I was beginning to think I would never get any answers. I have been seen by numerous doctors since I was 24 for these issues and nobody had any answers. Thank you for the article it helped a lot.
For 30+ years I have been dealing with chronic aching sensation on my left side that runs from my buttocks down through my knee and often times radiates into my abdomen and groin area, even making it difficult for me to catch a full breath at night. Over the years this sensation has worsened to the extent that my sons and wife stand, and even jump, on my buttocks and leg to provide my only relief (other than Ibuprofene which I prefer not to use on a regular basis). Recently, I visited my chiropractor who told me about the piriformis muscle and possible issues associated with the sciatic nerve. He said there is a possibility that my leg, stomach, abdomen, & groin issues may affected by the piriformis and recommended a few stretching exercises. After reading your web articles and applying pressure with my fist and now softball in the priformis area, I am convinced that this is what I have been dealing with all these years. After applying pressure to this area, amazingly, the sensation in my abdomen stopped, I could breath easily and the aching sensation down my leg disappeared. My mother in Pennsylvania also suffers from similar leg conditions for decades. I now plan to speak with my chiropractor about your treatments to see if he can provide a more permanent solution and I also plan to inform my mother about my findings at your website. I think you may have identified the potential culprits. Thank you so much! Hopeful in Phoenix.
I am an Australian, living in Australia, incapacitated by pain, I have learnt more about myself by reading this site, than I have learnt from any other medical practitioner or specialist.
I now see a ray of light.
Thankyou for taking the time, energy & compassion to put this site together. People in our situation NEED you.
BEEN LOOKING FOR SOMEONE WHO KNEW JACK BOUT FASIA AND NOBODY LISTENS. i HAVE FIBRO AS MY DAUGHTER AND PRETTY SURE MY SON AND OTHER DAUGHTER DO TOO. bUT IT FEELS LIKE A RUBBER BODY GLOVE THATS WAY TOO TINY ON BACKWARDS AND WITH TIGHT RUBBERBANDS ALL OVER. i ALSO CALL IT A STATE OF PARTIAL RIGIMORTIS BECAUSE i ALSO HAVE HEMACHROMOTOSIS AND i THINK IT HAS EVERYTHING TO DO WITH THE FIBROMYALGIA. i CAN NO LONGER LIFT ANYTHING WITHOUT PAIN. HAVE BULGING AND HERNIATED NECK DISCS. AND ARMS AND HANDS SO STIFF THEY WON’T STRETCH TO THEIR PROPER EXTENT. mY HUBBY SQUEEZES IT SO HARD BUT IT DOESNT BUDGE AND YOU THINK i WOULD BRUISE BUT DO NOT. i DON’T GET IT. i KNOW IRON DEPOSITS ARE UNDER AND BETWEEN THE FASCIA SOMEHOW BUT NOBODY LISTENS AND IT IS OXYGEN STARVED SOMEHOW FROM THE HEMO CUZ THE RED BLOOD CELLS CARRY THE OXYGEN AND IT EITHER GIVES US TOO MUCH OR TOO LITTLE AND IT STRANGLES OR RATHER SUFFOCATES THE FASCIA AND TISSUES CAUSEING THEM TO GET GRAINY AND HARD AND SCARED LIKE YOU ARE SAYING. WOW THANKS
Most informative!
This site was the most informative that I came across. It helped me immensely to understand more about Myofascial Pain Syndromes. Now I assist others in our massage class to have a better understanding. Cheers
What an informative site! Dr. Russell S. Schierling goes to great lengths to research chronic pain and has been helpful in assisting me find some relief in my hometown of San Jose, CA.
Thank you!!
Reina
I suffered what I thought was a minor, innocent, hamstring injury in fall of 2007 that just would not get better. I tried several different treatment routines and plans, all with no noticeable improvement. After talking with Dr. Schierling, he told be about the fascia tissue and the problems injuries like mine caused with the fascia. Long story made short, he said he could fix it, so obviously I was game! After two treatments a week or so apart, I noticed SIGNIFICANT improvement in my range of motion and strength capacity. Now, a short two months after the treatments and the follow up recommendations for my “at home” part of the treatment, I am now back to 100% capacity with my leg strength and flexibility. Thank You!
Thank you so much for your website! It really explains the Connective Tissue “Fascia”/Scar Tissue reasons for pain problems so often not known by most practitioners. After years of Doctor Visits, X-Rays, MRI’s (which showed nothing) and Failed Carpal Tunnel Surgery for “Repetitive Strain” pain problems in my Hands & Arms, your website is finally leading me in the right direction. God Bless you from Pittsburgh, PA.